The periodical of the Harley Street Medical Area Issue 11 / 2023
Gene genie
Clinical geneticist Dr Melita Irving on the challenges and rich potential of genetic medicine
T time
Understanding CAR-T therapy

Beyond the pitch Dr Jesus Olmo on his transfer from Real Madrid to Isokinetic
How does it work?
A guide to endoscopic aortic valve replacement

HCA UK CONCIERGE CENTRE LEADING YOU THROUGH YOUR HEALTHCARE JOURNEY For more information, please contact: E: enquiries.concierge@hcahealthcare.co.uk T: +44 (0)20 7616 4999 Our Rapid Response Referral service can co-ordinate your national or international transfer to an HCA Healthcare UK hospital. Our hospitals provide: • Acute and complex care • Intensive care • Orthopaedic care • Trauma rehabilitation • Neurological rehabilitation GLOBAL TRANSFERS TO/FROM THE UK REFERRAL RESPONSE WITHIN 2 HOURS 24/7 ACCESS TO CONCIERGE SERVICES TEAM
Prognosis is owned by The Howard de Walden Estate 23 Queen Anne Street London W1G 9DL 020 7580 3163 hdwe.co.uk
Estate contact
Annette Shiel annette.shiel@hdwe.co.uk
Publisher Lusona Publishing and Media Limited lusonapub.co.uk
Editor
Viel Richardson info@lusonapub.co.uk
Editorial consultant
Mark Riddaway mark@lscpublishing.com
Contributers
Ellie Costigan, Gerard Gilbert, Daphne Power, Christopher L Proctor, James Rampton
Design and art direction
Em-Project Limited
01892 614 346 mike@em-project.com
36 Beyond the pitch Dr Jesus Olmo of Isokinetic on the knowledge and experience brought from the world of elite football

36 Prognosis – 1
04 HSMA update
Mark Kildea on ensuring that the HSMA is equipped to play a leading role in the future of the UK healthcare sector

09 News
New arrivals, developments and events
10 Crystal ball
The evolution of treatments for presbyopia
11 Harley Street hero
Joseph Lister
12 How does it work?
Endoscopic aortic valve replacement
14 Thinking aloud
The thoughts of Maria Garcia, clinical director at All Points North London
16 Profile of a pathogen
Tuberculosis
18 How to Manage stress
20 A day in the life
Ryan O’Grady, head of pharmacy operations at Pharmacierge
24 From the ground up
Dr Nick Losseff of Cleveland Clinic
London on the privilege of building a hospital – and team – from scratch
26 Healthcare in the climate crisis
The potential of digital health
30 The big interview
Clinical geneticist
Dr Melita Irving on the challenges and rich potential of diagnosing and treating genetic conditions
36 Beyond the pitch
Dr Jesus Olmo of Isokinetic on the knowledge and experience brought from the world of elite football
42 T time
Doctor Mike Potter of The Royal Marsden on why CAR-T therapy holds so much promise
48 Q&A
Mr Alexander Bader of the Bader Medical Institute of London on the complex world of pelvic floor issues
52 Patient experience
Miles Ekersley on how Mako robotic hip surgery got him back on his feet
56 Service sector
Lina Patel of The London Clinic on combining clinical innovation with holistic care
60 My Marylebone
Aleksandra McNee, director of operations at Phoenix Hospital Group
62 What’s on Cultural events near the Harley Street Medical Area
63 Five Village food shops
64 The guide
Places to have a spa day in Marylebone
I entered the pharmaceutical profession to help people, but I hadn’t comprehended the complexities involved, and I hadn’t anticipated how the role of the pharmacist would continually expand.
Ryan O’Grady of Pharmacierge
20 2—Prognosis



56 30 48 16 Prognosis—3
HSMA UPDATE
Mark Kildea, chief executive of The Howard de Walden Estate,
The Howard de Walden Estate comprises 92 acres of Marylebone, central London which contains a vibrant neighbourhood of healthcare, residential, offices, retail and leisure, right in the heart of the city. With Harley Street, one of the most prestigious healthcare addresses in the world, at its heart, healthcare has always played an important role on the estate. This heritage is extremely important to us, but as with everything, healthcare moves on. Technology, for example, is having a significant impact. Over the past 10 to 20 years, The Howard de Walden Estate has continually studied this changing landscape to make sure that the area remains relevant and is recognised as a leader in the world of healthcare.
This is why in October 2022 we held
the latest in a series of conferences under the chairmanship of the Rt Hon Professor Lord Kakkar KBE, PC. Entitled London: A Global Hub for Life Sciences, it drew together important participants from healthcare, life sciences, business, property and law to discuss opportunities that exist for London to cement itself as an established location in the global life sciences arena, and the role the Harley Street Medical Area (HSMA) can play in this development.

Our philosophy at Howard de Walden is to stay relevant and purposeful, and while this requires that we recognise the area’s strengths, we also need to avoid being dominated by one use of our buildings. That’s why it’s important to have residents, shops, restaurants and offices, to create a vibrant community.

on ensuring that the Harley Street Medical Area continues to play a leading role in the future of the UK healthcare sector
4—Prognosis
Heritage is extremely important to us, but as with everything, healthcare moves on. Technology is having a significant impact. Over the past 10 to 20 years, The Howard de Walden Estate has continually studied this changing landscape to make sure that the area remains relevant.

Prognosis—5
What we want for Marylebone and our estate is forthis to be a great place to go for breakfast, lunch and dinner, and go out for the evening. But we also want it to be a great place to work and a great place to get healthcare services and treatments.
Healthcare takes place in buildings filled with expensive equipment and people in surgical gowns. It’s all rather clinical. The HSMA aims for something more welcoming. Key to this is how we refurbish and manage our buildings. We want to make sure they are purposeful for the 21st century and beyond, while working with their extraordinary architectural heritage.
Today, people are in hospital for very short periods of time. An increasing trend is for patients to pop in for a procedure and be discharged on that
same day. This has implications for the type of buildings healthcare operators need. Hospitals designed around the traditional longer stays have lot of beds, but will they need all those beds in the future? How do you transform a hospital of today to be the hospital of tomorrow?
Alongside the wonderful environment, one of the most important characteristics of the HSMA is the presence here of a high-quality skills cluster, something we are always looking to support. We have nursing skills, consultant skills, general practice skills and the ancillary services that support healthcare. HSMA occupiers benefit from the availability of labour as well as the attractiveness of the area. Medics like to talk to medics, they like to mix together socially as well
as professionally. We have a mature healthcare infrastructure in the HSMA that you don’t find in any other part of London. It’s also a name and brand that is well known and trusted around the world. If people want to see the best in a particular field, they head to Harley Street because that’s often where the best consultants are found.

A further consideration is the explosion of interest in life sciences in the UK and the greater conduct of research. In Harley Street, this is likely to intensify with the arrival of new entrants such as Mayo Clinic Healthcare, which build their success on the three shields: medicine, education and research. While several organisations such as the Sarah Cannon Institute and Re:Cognition Health actively run clinical trials in the HSMA, we think that the independent healthcare sector would benefit from more research. Having access to great local research facilities is a real advantage and we are working on ways to accommodate more research on our estate and build on the connection between healthcare and life sciences.
While the October conference identified several real challenges facing healthcare in the UK, there was a genuine optimism that with the right leadership and commitment those challenges can be met. We firmly believe that the HSMA can play a leading role in meeting these challenges.
23 Queen Anne Street London W1G 9DL 020 7580 3163 hdwe.co.uk
6—Prognosis
Alongside the wonderful environment, one of the most important characteristics of the HSMA is the presence here of a high-quality skills cluster, something we are always looking to support.
The Howard de Walden Estate

EXPERIENCE THE BEST OF UK HEALTHTECH AT ARAB
HEALTH
2023
30 January - 02 February 2023
ABHI hosts the largest and most visible group of UK companies at Arab Health. Our joint stand with the Department for International Trade is home to a busy four-day programme of live surgical simulations and dedicated partnering events. Be sure to visit Stand H2 D30 to learn more about the best in UK healthcare and HealthTech.

Arab Health by numbers

17 Country Pavilions
3,590 Exhibiting companies
55,000+ Healthcare and Trade Professionals
158 Countries Represented
NEWS
Harley Street Medical Area surgeons came together in November to perform both ‘live’ and simulated surgery at Future Surgery 2022. Organised by the Association of British HealthTech Industries (ABHI), the event’s simulated operating theatre gave surgeons a platform to demonstrate the latest pioneering surgical techniques to an audience of over 4,500 healthcare professionals. Visitors watched a wide array of cutting-edge demonstrations courtesy of some of the UK’s leading clinics and hospitals, including Moorfields Private Eye Hospital, Orthopaedic Specialists and The Harley Street Specialist Hospital.
futuresurgeryshow.com
Arab Health, the largest healthcare exhibition and conference in the Middle East, is taking place from 30th January-2nd February 2023 and The Howard de Walden Estate is pleased to confirm that the HSMA collective will be returning to the event for the sixth time. The team, which will include representatives of several of the area’s top clinics, will showcase their medical excellence on the HSMA stand within the UK Pavilion. Several members of the collective will also be talking at congress as part of the event.
arabhealthonline.com
Moorfields Private has added several new procedures to those available at its recently opened premises on New Cavendish Street. Patients can now choose the facility for cataract surgery, eyelid surgery (blepharoplasty) and glaucoma procedures. The site includes an operating theatre and a minor operations room for day surgery and intravitreal injections. It also offers ultrasound and has its own pharmacy. Andrew Robertson, director of private care, commented: “Moorfields is worldrenowned as a centre of excellence for ophthalmic care, and we are delighted to have extended our services in the heart of London’s clinical district.”
moorfields-private.co.uk
Isokinetic, a specialist sports medicine and rehabilitation group recognised as a FIFA Medical Centre of Excellence and as a reference point in the orthopaedic and sports rehabilitation sectors, has celebrated its 10th anniversary in the Harley Street Medical Area. An event held at the clinic was attended by the Isokinetic president Stefano Della Villa, CEO Marco Della Villa, and director of the education and research Francesco Della Villa, who all travelled from Bologna for the occasion. Andrew Massey, medical director at FIFA, was in attendance and gave a speech to mark the occasion.

isokinetic.com
The London Clinic and Fortius Clinic are among a group of independent healthcare providers who have donated more than a million medical supplies to Ukraine to assist in the ongoing crisis resulting from Russia’s invasion and occupation. Working in partnership with Ukraine’s UK embassy and the Independent Healthcare Providers Network (IHPN), the Harley Street Medical Area providers have been part of an effort to get items including anaesthetic machines, defibrillators, blood pressure pumps and first aid to areas in Ukraine where help is most needed.
ihpn.org.uk
King Edward VII’s Hospital has long understood the value of art in the rehabilitation process for patients and the promotion of wellbeing among staff. This can be clearly seen in the hospital’s partnership with the Zimmer Stewart Gallery, a collaboration showcasing an annually changing collection of 18 original paintings by six emerging artists over the six floors of the new King Edward VII’s Hospital Medical Centre. the crown of the hospital’s art collection has been an installation in the new outpatient centre by acclaimed abstract artist Bridget Riley.
kingedwardvii.co.uk

The Howard de Walden Estate hosted its annual Marylebone Christmas Lights switch-on event in November, a wonderful, uplifting occasion that brought the season of good cheer to children and adults alike. The highlight of the evening was broadcaster and author Fearne Cotton flicking the switch and bringing Marylebone’s dazzling display of lights and decorations to life. As well as raising spirits, the event raised a grand total of £15,000 for Howard de Walden’s charity partner, Mind.
hdwe.co.uk
Prognosis – 9
Isokinetic
King Edward VII’s Hospital
CRYSTAL BALL
Presbyopia
Dr Clare O’Donnell of Optegra on the evolution of treatments for a common eye condition
mid-range and close up vision. This gives you great all-round vision and the brain is excellent at selecting the part of the image you want to focus on. The surgeon uses a laser to create a temporary flap. They lift this and then with another specialised laser gently vaporise tiny amounts of tissue to reshape the cornea. Another approach is a refractive lens exchange, where we replace the natural lens with an implant called an intraocular lens. The great thing is that these lenses can be designed to correct prescriptions other than presbyopia, meaning they can correct life-long vision problems.
On the horizon
State of play
Presbyopia is the loss of the focusing ability of the eyes. Inside the eye we have a lens called the crystalline lens. When we’re young this lens is very flexible, which makes the eye very good at adjusting focus, but over time it can lose this flexibility. There are different theories as to why this happens – one is that the lens hardens, but it might also involve a deterioration of the muscles that control the focusing and relaxation processes. The traditional ways of addressing this are spectacles and contact lenses but these may not suit everyone.
Techniques such as Presbyond, a relatively new laser treatment for presbyopic patients, are designed to optimise the vision in one eye for mid-range and distance vision while optimising the vision in the other eye for
What I’m excited about is extending some of the technologies we have at the moment. We have a procedure called small incision lenticule extraction (SMILE). It’s sometimes called keyhole laser surgery, because instead of creating a flap and vaporising tissue, the surgeon uses a single advanced laser to create a ‘lenticule’ of tissue within the cornea, which is then removed through a tiny opening no bigger than the tip of a pen. That simple process is enough to reshape the cornea and correct the patient’s vision. It is a very safe and effective procedure but at the moment it is not suitable for presbyopia, especially for those who may have other issues as well. But I’m sure the day it becomes suitable is not far away.
Another approach with a great deal of potential is called an implantable collamer lens (ICL). Behind the iris, a lens is implanted containing the optics required, correct to the patient’s distance prescription and reading prescription. It’s
A
beneficial impact of all lens replacements treatments is that the new lenses do not develop cataracts over time, a major cause of visual impairment and even blindness. This has been a big step forward.
a very safe procedure that’s been around for a number of years now. We have only recently developed the lens technology to offer treatment to people suffering from presbyopia. However, there will undoubtedly be further developments in the range of lens designs and prescriptions available in the future.
In the distance
I guess the holy grail would be dealing with the loss of flexibility of the crystalline lens, either by softening the lens or re-engaging the muscles that control the focussing mechanism. There is currently research underway into creating lenses that behave much more like our natural lenses. These are called ‘accommodating implants’ and have the flexibility and dynamic abilities of the eye’s natural lens. There have been many attempts to deliver this technology, and while you never know what is going on in research laboratories, it’s probably fair to say that we are some way away from that at the moment. However, I have no doubt that we will eventually achieve these breakthroughs. A hugely beneficial impact of all lens replacement treatments is that the new lenses do not develop cataracts over time, a major cause of visual impairment and even blindness. Developments in implant technology have been a big step forward for the estimated 2.1 billion people worldwide who suffer from presbyopia, and these improvements are sure to continue.
10—Prognosis
Optegra 25 Queen Anne Street London W1G 9HT 0800 077 3727 optegra.com
hugely
HARLEY STREET HERO Joseph Lister

1827-1912
Surgeon
Words: James Rampton
Image: Wellcome Collection
In the whole of London, only one surgeon in history has been honoured with a statue: Joseph Lister. The monument to the doctor known as “the father of modern surgery” occupies a prominent position in the middle of Portland Place, hard by Harley Street. There is also a statue dedicated to Lister in Kelvingrove Park in Glasgow, and the Lister Hospital in Chelsea is named after him, too.
So, why is he so celebrated? The answer lies in the fact that medical history is split into two very distinct eras: pre-Lister and post-Lister. His work on antiseptic surgery changed the face of medicine forever.
Before Lister published his theories on sterile surgery, it was generally thought that infected wounds were the result of chemical damage caused by fetid air. As a result, surgeons did not routinely wash their hands or equipment before operating.
However, Lister, who was born in West Ham in 1827 and later in life lived very close to Harley Street at 12 Park Crescent, became convinced that sterile surgery was the only way to prevent the spread of infection. In a major breakthrough, he linked Louis Pasteur’s ground-breaking germ theory of fermentation to putrefaction in wounds.
On 12th August 1865, Lister’s theories were proven for the first time. Working at Glasgow Royal Infirmary, he applied full-strength carbolic acid as a disinfectant to the wound of an 11-yearold boy called James Greenlees.
Greenlees had suffered a compound fracture in his leg after being run over by a cart. Six weeks later, Lister was astounded to find that the boy’s
bones had healed without any sign of suppuration.
Between March and July 1867, the surgeon wrote six articles for The Lancet detailing his trailblazing results. These astonishing discoveries reduced the number of post-operative infections and ushered in an age of far safer surgery. It is not hyperbolic to suggest that Lister’s findings saved millions of lives.
After the publication of Lister’s Antiseptic Principle of the Practice of Surgery in 1867, his leading-edge techniques were exported all over the world.
For instance, in 1869, Mathias Saxtorph from the University of Copenhagen came to Glasgow to learn about Lister’s methodology from the master himself.
The following year, Saxtorph wrote a letter to Lister acknowledging the difference his new-found skills had made to his patients. “The Frederick Hospital, to which I am head surgeon, is a very old building, and I have 150 patients in the surgical wards,” he explained. “Formerly, there used to be every year several cases of death from pyaemia [blood poisoning], sometimes arising from the most trivial injuries. Now, I have had the satisfaction that not a single case of pyaemia has occurred since I came home last year, which result is certainly owing to the introduction of your antiseptic treatment.”
Lister, who was made president of the Royal College of Surgeons in 1895, and elevated to a baronetcy in 1897, continued to break new ground up until his death in 1912. He was, for instance, the first surgeon in Britain to utilise
a rubber drainage tube. His patient? Queen Victoria.
In March 1900, Lister was appointed serjeant surgeon to the Queen, the senior surgical post in the Royal Household. He carried on in the role after Victoria passed away in 1901, serving her successor, King Edward VII.
Lister’s services were urgently called upon the following year. On 24th June 1902, after 10 days of excruciating appendicitis, the monarch was wheeled into theatre for an emergency operation. The appendectomy was conducted by Sir Frederick Treves, another famous former resident of the Harley Street area. The date? A mere two days before Edward’s coronation.
The operation was one that came fraught with peril. The King faced an exceedingly high danger of dying from post-operational infection. For that reason, no doctor would risk carrying out the operation without first seeking advice from the world’s most distinguished surgical authority.
Even though he had retired in 1893, Lister was still very much at the top of his game and informed Treves of the most up-to-the-minute advances in antiseptic surgery.
Treves obeyed every comma and semi-colon of the eminent surgeon’s advice and Edward lived. Lister had once again reinforced his reputation as the doctor who revolutionised the safety of surgery.
In the aftermath of his successful surgery, Edward VII told Lister: “I know that if it had not been for you and your work, I wouldn’t be sitting here today.”
Perhaps you could say the god-like surgeon saved the King.
Prognosis—11
HOW DOES IT WORK?
Endoscopic aortic valve replacement
Mr Toufan Bahrami, senior cardiac consultant surgeon at Royal Brompton & Harefield Hospitals, on a pioneering endoscopic cardiac procedure that delivers significant benefits for the patients
Interview: Viel Richardson
The aortic valve is a structure in the heart that sits between the ventricle and the aorta. In a healthy heart, oxygen-rich blood is pumped from the ventricle chambers through the aortic valve into the aorta, which then distributes the blood into general circulation. The aortic valve has three flaps called ‘leaflets’ which open each time the heart pumps to let blood flow into the aorta. They then close, sealing the valve to prevent any flow back into the ventricle.
There are two main disease conditions that might lead to someone needing a valve replacement. One is aortic valve stenosis, where the valve becomes narrowed and the leaflets cannot open fully. Instead of an opening of around 1.5-2.5cm, it might be around 0.6-0.9cm, meaning the heart has to work much harder. With stenosis, the leaflets can also become calcified, losing their flexibility. They are usually so thin and flexible they appear transparent, but once calcified they’re like wood, with very restricted movement, meaning they don’t make an effective seal to stop blood flowing back into the ventricle.
The second disease is aortic valve regurgitation or leakage. With this, the leaflets have normal flexibility but the ring holding the leaflets is dilated, so they don’t close properly. A leaflet can also become too flexible, so the seal is again compromised and blood can get back into the ventricle
The traditional and still most common approach to aortic valve replacement is a sternotomy. This involves making a 20-25cm incision down from the top of the sternum. We then use retractors to spread the ribs apart. This allows us to
gain access to the heart and place the cannula tubes that go to the heart-lung bypass machines needed during the procedure.
A sternotomy is a major operation. We are creating a large opening of the chest cavity and a significant displacement of the ribs, and this leads to problems even after a very successful procedure. Patients can suffer from serious back and neck pain or pain in the ribs. They often have some difficulty breathing. This all means a long stay in hospital and a slow recovery. It can take the patient several months to get back to a fully active life.
There is also the option of a ministernotomy, which is the same as the standard treatment, but done through a smaller opening. The recovery time is a little better, but you still have most of the issues of the full sternotomy. There have been other attempts to limit these issues, but I decided to try a completely different approach.
Ventricle chambers The heart has four chambers. The top two chamber are the right atrium and left atrium. The bottom two chambers are the right ventricle and left ventricle. Each of these chambers has a valve that keeps blood flowing in one direction.
Leaflets Flaps of tissue that make up the aortic valve. They act as one-way inlets for blood coming into a ventricle and one-way outlets for blood leaving a ventricle.
Minimally invasive A form of surgery performed through one or more small incisions, using small tubes, tiny cameras and surgical instruments.
Catheter A flexible tube that is inserted into the body, allowing liquid to flow to or from an organ.
12—Prognosis
I have been a minimally invasive endoscopic surgeon for 22 years and at every stage of cardiac surgery I have tried to be less invasive in my work, as I have seen the benefits this brings to patients. I started developing a technique through which I could replace the aortic valve with a fully endoscopic procedure, therefore avoiding opening the ribcage and the trauma this causes. For the past two years, I have been doing the procedure totally endoscopically. All that’s need is a soft tissue opening about 3cm wide for the procedure and another opening on the side of the chest for us to insert the camera. The whole operation is done on the screen, similar to robotic surgery. This is the only centre in the UK where this procedure is carried out.
First, we carry out a very detailed investigation using equipment such as high-resolution CT scanners to create 3D reconstructions of the area. The idea is to spot any potential complications and create a clear plan before starting the procedure. For the operation itself, we make those two small incisions –the opening for the new valve and the surgical instruments to go through and the incision for the camera. We use the groin vessels in order to bypass the
heart function, so there is no need for catheters in the chest area.
Once inside, we cut away the damaged or calcified tissue to create room for the new valve. After the area has been prepared, we insert the replacement valve, which can be made from either tissue or metal, and suture it in place. The whole operation takes about two to three hours.
It is a very different operation from a sternotomy. It requires new skills. You operate with much longer instruments – 30cm instead of 10-15cm. The surgeon works while looking up at the screens, not down at the heart. That takes training and experience. But the view the screens give you is so much better than looking at the heart directly, as you can manipulate both the camera and the image to get precisely the angle you need.
This a personal opinion, but I think the result is much better. The clarity of view you get on the screen is so superior that I believe it improves the quality of your work, as long as you have been properly trained in endoscopic surgery. Also, we are achieving the introduction of a new valve through a 3cm opening and not a 30cm one, which is better. With the full sternotomy, patients are
often not woken until the following day and then spend two to three days in intensive care, then time in a recovery ward before going home. My patients often go home about four days after the procedure.
I’m passionate about this procedure because I have seen what it does for my patients, especially during their recovery. I have performed both types of procedure and at three weeks, for example, there is an incredible difference between the two. I have mentioned the problems such as back pain that sternotomy patients can suffer from for months afterwards – many struggle to walk for more than 10 to 15 minutes a day as they build their fitness back up. With endoscopic surgery, it is a completely different story. At three weeks some are back to work, they start driving again, they are fully active and getting their fitness back. One patient in his sixties send me a picture of himself hiking in the Pyrenees. It was remarkable.
Royal Brompton & Harefield Hospitals Specialist Care
77 Wimpole Street, London W1G 9RU 020 3553 9648
rbhh-specialistcare.co.uk
Prognosis—13
Sternotomy Endoscopic aortic valve replacement
3cm opening for procedure
3cm camera access
To heart bypass machine
Specialised endoscope with surgical tools
To heart bypass machine
Sternal retractor used to separate ribs
THINKING ALOUD
Maria Garcia, clinical director at All Points North London

Interview: Ellie Costigan
Addiction appears hand in hand with poor mental health. There are different theories as to why, but there is evidence to show that there are high rates of comorbid substance use disorders and anxiety disorders, as well as depression, bipolar disorder, attention-deficit hyperactivity disorder, psychotic illness, borderline personality disorder and antisocial personality disorder.
A thorough assessment is required to ascertain whether the addiction or the mental health disorder should be addressed first. Generally, if the addiction is severe, this should be treated first, as otherwise it will continue to be a block to any progress and recovery on the general mental health side of things.
14—Prognosis
By bringing so many aspects of treatment under one roof, APN reaches across imaginary boundaries and healthcare silos to offer the full continuum of care – anytime, anywhere – ensuring long-term success for clients.
When we first opened All Points North in the US, the majority of our clients were flying in from the UK, Europe and the Middle East, which demonstrated a need for more accessible mental health in those parts of the world. APN London will provide continuity and consistency of outpatient care for UK patients returning from their treatment at the APN Lodge in Colorado.
Harley Street is a hub for the UK’s behavioural health sector, and we are pleased to call London our first UK home. The new clinic is set within a beautiful Georgian building on Wimpole Street, split across several floors, which has been renovated to accommodate the comprehensive, multidimensional mental health services we offer, for mind, body and soul.
It’s estimated that 40-60% of individuals relapse while in recovery. At APN, we recognise that we cannot produce better outcomes by trying the same tired old techniques. We believe that by adopting new technologies and emerging evidence-based treatments without fear, the industry can better support and treat people throughout their journey to lasting health.
We shepherd people through the entire treatment process: from the very first call to the contact centre, where a real person – likely someone who’s in recovery themselves – will introduce you to a robust social club through which you can make connections with others who are pursuing good mind and body health.
At All Points North, we support a person through their whole journey. People are often at their most vulnerable when they come to see us, so we encourage our staff to take an iterative approach to find the right solution. Rather than a one-size-fits-all approach, we offer integrated care and custom treatment plans to help everyone find their own ‘true north’.
Prognosis—15
All Points North apn.com
Mycobacterium A genus of over 190 species of bacteria. This genus includes bacteria that cause serious illnesses such tuberculosis and leprosy.
Hominid The group consisting of all modern and extinct Great Apes. The includes modern humans, chimpanzees, gorillas and orang-utans plus all their immediate ancestors.
Tubercle bacillus The small, rod-shaped bacterium that causes tuberculosis.
Monoarticular joint pain Pain isolated to a single joint.
Meningismus A group of symptoms similar to meningitis (stiff neck, reaction to light and headache), without inflammation of the membranes lining the brain.
PROFILE OF A PATHOGEN
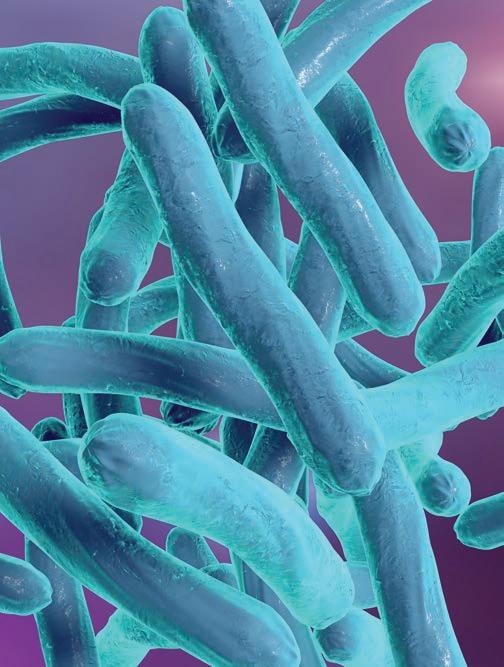
Tuberculosis
announced that he had isolated the tubercle bacillus. This discovery was followed by the development of the Pirquet and Mantoux tuberculin skin tests, Albert Calmette and Camille Guérin’s BCG vaccine, and antituberculous drugs like streptomycin. Yet in 2018 an estimated 1.5 million people died from the disease and in 2021 an estimated 10.6 million people contracted it globally.
Tuberculosis (TB), a highly infectious disease caused by a rod-shaped Mycobacterium tuberculosis (MT), has been lurking on the fringes of humanity’s story for millennia. It has been hypothesised that the genus Mycobacterium originated more than 150 million years ago and that an early progenitor of MT may have been abroad among early hominids in East Africa. What we do know is that TB has had time to reach every corner of the globe. According to a World Health Organisation report, in 2022 the disease was reported in territories containing more than 99% of the world’s population. It’s everywhere.
As far back as 1720, the physician Benjamin Marten conjectured about person-to-person transmission of the disease. In March 1882, Robert Koch
There are two basic types of tuberculosis: pulmonary and extrapulmonary. Pulmonary tuberculosis takes hold in the lungs. Symptoms can include a bad cough lasting three weeks or longer, tightening of the chest, night sweats, weight loss, fatigue, pain in the chest and the coughing up blood or phlegm from deep inside the lungs. But the disease can also spread to other organs, resulting in extrapulmonary tuberculosis (EPTB) which is on the rise. Organs affected can include the central nervous system, eyes, lymph nodes, musculoskeletal system, genitourinary tract and gastrointestinal tract. With EPTB the symptoms depend on the organ infected, making it difficult to spot. Sufferers may present with abdominal pain, diarrhoea, infertility, monoarticular joint pain, headache, meningismus, or lymphadenopathy. Tuberculosis is particularly dangerous for people living with HIV, which must be taken into account during an outbreak.
The bacilli are spread by infected airborne droplets, making TB extremely contagious. Once a person is exposed it can take three to nine weeks for the symptoms to appear. However, it can

remain as a latent tuberculosis infection (LTBI) for years before the disease breaks out. The good thing is that people with LTBI are generally not infectious. However, once the disease is established patients can remain infectious for two to three weeks after treatment starts.. For this reason, tuberculosis is a ‘notifiable’ condition, which means that local health authorities must be informed in writing within five days of a confirmed diagnosis or suspected case.
The bacteria can be detected by two tests: a TB skin test (TST) such as the Mantoux skin test, and TB blood tests such as interferon-gamma release assays (IGRAs). However, these only detect the presence of the bacteria, and cannot tell whether the person has LTBI or has progressed to TB disease. Other tests, such as a chest x-ray and a sample of sputum, are needed to confirm this.
There are several potential treatment regimens, all of which can last for between four and nine months – not a quick fix. Also, TB has developed resistance to some antibiotics, meaning that any treatment path must be modified if the patient has been in contact with an individual with drugresistant TB.
Tuberculosis has been with us for so long it can almost be seen as part of being human. But we are making progress. For most of its history, tuberculosis has been associated with a high mortality rate, and untreated this is a very dangerous disease, but modern treatments are highly effective if delivered in time. The hope is that one day a disease that has stalked us for as long as we have walked the earth will eventually be consigned to the history books.
16 – Prognosis





HOW TO MANAGE STRESS
We all experience stress, but what are the symptoms that suggest it might be time to go to the doctor?
It is important to look at stress as a cycle. Stress is cumulative and can be carried over if not processed. If you feel that it’s unremittent or you cannot cope with it, those are the signs that stress is beginning to mount, and that accumulation of stress can cause a wide variety of issues. People can be in a hyper-vigilant state before bed, which affects their sleep. You might develop recurring infections. Underlying health conditions might flare up for no obvious reason. You could experience gut issues – symptoms similar to irritable bowel syndrome – and in women, it can disrupt the menstrual cycle. It can also affect sexual activity. You might experience heart palpitations or have tension headaches. But if we are able to recuperate, process, release or work through the stress response then we can avoid developing any of the harmful effects of a chronic stress state.
Is there are an emotional component to it as well?
Yes, there’s an important emotional component. You might find you no longer have access to higher emotional states, such as joy, or feel unable to regulate your emotions, becoming impatient and struggling to communicate effectively or to feel compassion or gratitude. This can in turn bring on low-grade anxiety and depression. In short, long-term high stress affects every single system in your body, and everybody will react differently.
Are there any long-term health effects?
Our body does not differentiate between real and perceived stress. If a lion walks into the room, the body detects a threat, and it will change your physiology, so you are ready to fight, run or freeze. Your blood pressure and blood sugar will rise, there will be an increase in muscular tension. The problem is, the same thing happens if you get an unexpected email from your boss, for example – but in that case we don’t run or fight, so that energy gets suppressed. A day or year of that isn’t a problem, but over time you could develop hypertension, coronary heart disease or diabetes. When we’re in a state of stress, our immune system is directed away from fighting off disease, so if that’s consistent, it can lead to autoimmunity problems or cancer – not to mention mental health issues, such as anxiety and depression.
How do you treat those patients?
The first thing I do is help you redefine how you see stress. People assume it’s bad, but stress can also be good or neutral. Getting married can be stressful, for example, but is a good thing – hopefully! There are two aspects to think about: your internal state and your external environment. Sometimes it’s about adjusting the external – if you’re in a toxic relationship or suboptimal work environment, for example. The internal is more about how you’re living your life. Are you on autopilot? Are you repeatedly engaging in behaviours that are not serving you? Are you energetic? Because you should be. Sometimes, we have to look backwards
before we can look forward. It’s also useful to look at who we model our stress response on, as it’s not something that is taught.
Is it possible to address the symptoms of stress?
To address these symptoms, we can engage in active relaxation, awareness of patterns and reframing. For a deep dive and holistic approach, I run the six-to-eight-week Harvard stress management and resilience training (SMART) programme. This empowers people to leverage neuroscience in managing stress effectively through mind-body practices.
Can you give us some examples of active relaxation?
The biggest thing is prioritising sleep, because it’s the most powerful reboot we have. Movement is also important. That could be getting up and having a stretch, going for a walk, or more moderate-to-intense exercise. Third, pay attention to what you’re putting in your body, including hydration. To promote relaxation, the best thing to do is stimulate your vagus nerve. This can be done through movement, breath work, cold immersion such as wild swimming or a cold shower, singing, humming or laughing. Journaling has also been shown to be good for relaxation – as is connecting with others.
How does laughing help?
When we belly laugh, we’re forcing ourselves to breathe, which engages our diaphragm. This is where the vagus nerve sits.
Are these things that all of us should be doing?
I’m very in favour of embedding strategies into our everyday lives. Bookend your day, so start it and end it right. If you have five minutes in the morning, get up, do a stretch or two, take a few really deep breaths, or have a 30-second cold shower. Think of one thing you want to accomplish that day to boost dopamine and one thing you’re grateful for to boost oxytocin. Put on a song and dance for three minutes. It really doesn’t take much. Start small, with whatever you’re able to do, and build it into a habit.
18 – Prognosis
Mayo Clinic Healthcare 15 Portland Place London W1B 1PT 020 7871 2575 mayoclinichealthcare.co.uk
Dr Safia Debar, general practitioner at Mayo Clinic Healthcare Interview: Ellie Costigan




A DAY IN THE LIFE
Ryan O’Grady
Head of pharmacy operations at Pharmacierge
Interview: Daphne Power
There is lot more involved in the daily running of a pharmacy than you might expect, particularly one as unusual as Pharmacierge. This is a family business that has been supporting patients and clinicians in the private practice arena for over 50 years. The culture is a personable one – it’s about treating patients as family – and the pharmaceutical offering has a variety and diversity of medications rarely seen elsewhere. These were the factors that led me to join the business three years ago.
I entered the pharmaceutical profession to help people, but to some extent I thought I’d probably just be signing boxes of tablets for the rest of my life. I hadn’t comprehended the
complexities involved, and I hadn’t anticipated how the role of the pharmacist would continually expand.
I’m usually in Wimpole Street by 8.30am. The first thing I do is meet up with the team and address any enquiries that have come in or concerns that have arisen. After that, as part of the management team it’s my responsibility to assess the state of the pharmacy. That means looking at how many prescriptions we’ve received and how many we need to send out, dealing with the queries that have come in, then helping to get the medications prepared, assembled and checked by a pharmacist – either me or one of the other 10 who work here. One of my most important
responsibilities is ensuring the medication and prescriptions are clinically screened and that everything is aligned with the many regulations that govern what we do.
After those initial checks and assessments, I will spend the day working closely with our teams in all different areas of the pharmacy and dealing with clinical enquiries. A clinician will often ask whether we can obtain a particular medication. With some pharmacies, if they don’t have it, that’s where the conversation stops, but for us that’s where the conversation starts. We will proactively source that medication.
Sometimes, it will fall to me to do this, but often the lead will be taken
20—Prognosis

Prognosis—21 w
Much of the work I do revolves around medication shortages, which have been cropping up a lot recently. For instance, HRT medication has been very hard to source this year. We’re working to source the medication where possible but also liaising with our clinicians to offer alternatives.
clinical information and clinical data. Our aim is to find a resolution for the patient in a structured manner and within a timeframe that suits them.
by our founder, Leon Ungar, who has a longstanding relationship with many suppliers and factories. Sourcing drugs that are perhaps less widely used is something we pride ourselves on. For me personally, it’s incredibly interesting to find out about novel, cutting-edge medications. It’s an ongoing educational experience which I find incredibly rewarding.
Much of the work I do revolves around medication shortages, which have been cropping up a lot recently. For instance, HRT medication has been very hard to source this year. We’re working to source the medication where possible but also liaising with our clinicians to offer alternatives. If there is a national manufacturing delay, as has occurred with the HRT product, we will try to suggest alternatives based upon
We are not your standard high street pharmacy, so while some of our patients do occasionally come in to see us face to face, mostly we communicate by phone or email. The first we know about the patient is from their prescription, but then subsequently we will have conversations and requests for information and advice, which we’re always on hand to provide. This could be related to the administration of a new medication, or I might have a chat with a patient who wants to know why their doctor has moved them from one medication to another and is keen to understand the differences. Patients are becoming more and more curious about pharmacology. As 99% of what we do is prescription only, we don’t have people walking in asking about coughs or colds. The advice we give will relate directly to a patient’s prescription.
Couriers deliver our medication throughout London and as far afield as Scotland, Wales and Cornwall, with prescriptions being collected from our pharmacy in Wimpole Street. We liaise with patients to ensure the delivery time is suitable for them.
During the pandemic we were presented with a whole load of new cases where people were stranded, not just in the UK but in Europe and across the world. We had a request from a dermatologist in Cambridge who had a patient who normally would have been in the UK but was stuck in Andorra and
in need of their medication. It was a rare cold-chain biologic which was not something we had dispensed before. We got in touch with the manufacturer directly to ensure we could receive the supply and then figured out a way to get it to Andorra without it rising above a temperature of 8°C. In the end, we commissioned a refrigerated van to drive it across Europe to the patient. That’s not something we do every week, but it illustrates the kind of challenges we faced during the pandemic and underpins our commitment to always going the extra mile.
More recently, we’ve had situations when patients have run out of their medication, or don’t have it with them, for whatever reason. Because of the excellent relationship we have with our clinicians, we can get prescriptions arranged for patients really quickly.
Looking to the future, we’re keen to continue developing the technological side to our pharmacy, possibly be delving into AI, to increase efficiency and delivery. But none of that would ever replace our oversight of the regulatory requirements of the pharmacy, nor the personal touch that’s so important to us. Some patients have been with us for decades – 30 years plus. Maintaining those relationships with the patients and clinicians is at the core of what we do.
8 Wimpole Street
London W1G 9SG 020 7631 1269 pharmacierge.com
22 – Prognosis
Pharmacierge
“Nobody understood my eyes more than Moorfields.”






Glasses and contact lenses didn’t fit into Evgeniya’s active lifestyle, leading her to feel she was missing out. After laser surgery, she’s not missing out anymore.
“I have worn glasses ever since I was in high school, before switching to contact lenses due to my active lifestyle. But contact lenses gave me dry eyes and glasses weren’t practical for me - I wanted to be able to see better when going about my daily life. I spoke to a number of companies offering vision correction but, due to an issue with my cornea, I didn’t feel comfortable having the procedure with them. Then I went to see Moorfields Private. They were able to assess my eyes and find a solution I feel I would not have found anywhere else. My surgery has improved my quality of life incredibly. I enjoy my daily activities more and I no longer feel like I am missing out on life.
I feel a lot safer, especially when driving, as it’s improved my peripheral vision. I don’t remember ever being able to see as well in my life. I wish I’d done it sooner.”
For over 200 years Moorfields has pioneered research, employed the brightest minds, and delivered visionary eye care. We offer the full range of ophthalmic care including cataract, vision correction, glaucoma and complex eye conditions.

To find out more or book your consultation: Visit moorfields-private.co.uk/contact-us Or call us 0800 328 3421 (Monday – Friday, 8am – 6pm)


Find us at: City Road EC1 New Cavendish Street W1
FROM THE GROUND UP
is very much built around easing a patient’s dealings with diverse teams and services.
This is one of the most digitally advanced hospitals in the UK. Our digital systems are underpinned by our electronic medical record, EPIC, which represents an enormous step forward in patient safety. This brings everything about patients together in one place that’s easily accessible by our caregivers, the patients themselves and the consultants who have referred their patients to us. All communications, radiology, laboratories and orders are in one place. This is particularly beneficial for those patients who have multi-disciplinary needs, because having a shared record speeds up the communication process and means we can share information seamlessly. We’ve also got an intensive care unit that is staffed by a consultant intensivist all day every day.
who want to work collaboratively.
Interview: Ellie Costigan
We opened our medical outpatient building on Portland Place in September 2021. Then, in April 2022, we opened the hospital on Grosvenor Place. It’s very exciting to be offering Cleveland Clinic care in the United Kingdom. Of course, there are meaningful interactions between us, Cleveland Clinic London is not simply a franchise of the North American organisation. With these facilities, we are building an international clinical network that opens patients up to that global expertise, rather than having it contained in London.
I’ve spent many years looking after international patients and I know what the issues are – they’re coming a long way, into a strange environment in which they may not completely understand the culture. We need to make that journey as comfortable as possible, which includes recognising the fact that people may only be in London for a short time. You need to coordinate opinion from multiple specialists as quickly as possible. Their treatment may involve dealing with health offices, embassies and sponsors, who often have different foibles to private medical insurance companies. The development of our global patient services team
One of the major benefits of our model is that it’s a group practice. Often people work in silos but here we have real integration of teams, both within departments and across specialities. This means different departments are able to work together seamlessly. Most of us are employed by the organisation. I don’t see patients and charge them for my services, I get paid a salary This means that surgeons are free to take on complex cases where the patient may find it difficult to find insurance cover for.
There’s a research and education element to what we do, too – we’re the first private hospital to sign a systematic training contract with a London medical school. This shapes our environment and ethos. We run a lot of portfolio studies, which puts us at the cutting edge.
All of those things come together to provide a better environment for us to work in, and a better environment for patients. Patient care is about so much more than technical skill – it’s about the team surrounding them, the pre-operative assessment, the post-operative management, the ICU management, the rehabilitation. Patient care is tangibly embedded into our organisational structure.
One of the overarching things Cleveland Clinic wanted to do here in London was combine the best of US and UK medicine. I think doctors in the UK have a more clinical approach to patients than other countries, because there are relatively few doctors per capita compared with Europe. This means they have enormous and extremely broad clinical experience but haven’t
necessarily had access to the latest technology – certainly in the public sector. It’s been our mission to combine those things, and I hope we’ve achieved that.
It’s been a unique opportunity to build a hospital from scratch, which is no small undertaking. I’ve developed a lot of stroke services in the NHS, and it can take years to develop a unit to maturity within an established hospital or change an existing system. Building something from nothing has been huge fun – and seeing people coming in now and beginning to benefit from it is enormously stimulating, as has been the opportunity to get to know so many other physicians who want to work collaboratively. All the doctors I’ve met throughout the project are good, sensible people who I can work with harmoniously. That’s been consistent, which is just fantastic.
But the best part of my job is always seeing patients. Wherever I’ve worked, that hasn’t changed. It’s a great privilege.
24—Prognosis
Dr Nick Losseff, consultant neurologist and head of global patient services at Cleveland Clinic London, on the privilege of building a hospital – and team –from scratch
Building something from nothing has been challenging but it has also been huge fun – and seeing people beginning to benefit from it is enormously stimulating, as has been the opportunity to get to know so many other physicians
Cleveland Clinic London 24 Portland Place London, W1B 1LU 020 3423 7500 clevelandcliniclondon.uk

Prognosis—25
HEALTHCARE IN THE CLIMATE CRISIS
The global impact of climate change on healthcare – and vice versa – is vast. In this series, experts from within the diverse community of the Royal Society of Medicine offer their unique perspectives
THE POTENTIAL OF DIGITAL HEALTH
Loy Lobo, a former president of the RSM’s Digital Health Council, and Dr Tim Ringrose, who currently fills that role, explain what ‘digital health’ means and the contribution it can make to achieving the NHS Net Zero target
Loy Lobo
Digital health is a fairly loose term that has evolved significantly during my time at the Royal Society of Medicine. In 2015, the council covering the area was called the Telemedicine and eHealth Council. A few years ago, this was renamed the Digital Health Council because so much was happening that went beyond the concepts of telemedicine and electronic health records. This included the large-scale collection and analysis of increasingly sophisticated data, and the use of that data for clinical decision support, all of which is incorporated under the umbrella of digital health. So too is the creation of medical devices that are increasingly software and data driven. In fact, the notion of digitisation in healthcare is impacting almost every aspect of healthcare you could imagine.
For me, a digital health system requires the application of three things. One is ‘design thinking’, which is really important as a way of re-imagining and reshaping health services. The other two are the sophisticated use of data and the effective use of digital technology. These three elements come together to either reshape existing services or create entirely new ones.
One of the most important words here is ‘effective’. Our health system was set up in the middle of the last century and it is clear that we need to redesign it to address modern health issues. Digital health services are playing a key role in that transformation, which is taking place at two levels. One is the formation of integrated care systems (ICS). I feel optimistic that providing accountability and budgetary responsibility to commissioning services at this level will lead to better integration.
The other aspect is the design and deployment of health services with a location-based approach. You divide the overall health system into place-based localities and then develop services that meet the needs of the population that live and work there.
The application of digital services capabilities would undoubtably help enable the reshaping of these services. There are some things that need to be agreed at a national or regional level – for example, setting the style and format of electronic health records used across areas such as primary care, social care, acute, community and mental health settings. The systems we select for each of these care settings would be fully able to share data with each other. With this in place, the local health providers would
26 – Prognosis

Prognosis – 27 w
have the requisite freedom within that framework to design services for the local community. So, for example, a domestic abuse tracking and prevention system in the centre of a major city might look very different from one in a small rural community.
For me, the words that best encompass what an effective digital health system offers are ‘flexibility’ and ‘integration’. We need to create a flexible system that serves the needs of an increasingly diverse society which faces issues that are not the same as they were 70 years ago when the NHS was created. We are now dealing with many more people who are managing long-term conditions like diabetes and hypertension, and the system was not designed for that. It is changing, but we are not there yet. Digital health is the means by which we create a National Health Service with the flexibility and capacity to meet the needs of our present and future population.
Dr Tim Ringrose
As president of the Digital Health Section, my role is to facilitate collaboration with other RSM sections about how digital technology can support all aspects of healthcare.
I think introducing an effective digital health system can place a key role in helping the NHS meet its Net Zero targets in a number of ways. It is commonly said that 5% of the traffic in the UK is generated by the NHS – things like patients’ journeys to and from appointments, doctors travelling for work, supplies and logistics, the vehicle fleet. The Royal College of Physicians recently produced a paper saying
that the NHS produces more carbon emissions than all of the flights in and out of Heathrow every year.
That is an enormous number, and while there are some obvious solutions, like electrifying the vehicle fleet, I also think the advance in digital technology brings with it huge potential. How many of those trips could be avoided altogether? The RCP also surveyed hospital doctors and found that about 10-20% of the patients they see in outpatients units don’t really need the appointments – they could be effectively treated without that trip to hospital. This is important because if you exclude emergency departments, 85% of a hospital’s activity is outpatient appointments. Even if we take the lower figure of 10%, reducing this offers a huge opportunity to change.
There are already some services that help to reduce this. One, called Consultant Connect, has an online portal that allows GPs to get pre-referral advice or have images reviewed by a consultant in the appropriate field when deciding to make a referral. If they make the referral, the service saves an enormous amount of time by preventing patients from attending appointments only to be told they need to see another specialist or they need to take specific tests before a diagnosis – all of which happens quite often at the moment.
Another large cause of unnecessary emissions is the 10-20% of outpatient appointments that are missed. People talk about charging for missed appointments, but we really need to tackle the root cause. Many appointments are missed because people are sent a letter saying they have
to attend at a specific date and time. If they can’t attend, it can be very hard to change the appointment, so many people just think: “Oh well, I can’t go”. In the rest of life, we’re used to being able to book things online. For those patients who have the facility to make electronic bookings, it makes sense to contact them offering a choice of dates and allowthem to pick the most convenient. This is an exciting time because people are beginning to understand the enormous possibilities of AI. It’s now entirely possible for an AI program to listen to a consultation and make medical notes in real time. But it goes far beyond just transcribing a conversation. It could quickly retrieve results of past tests when asked and produce a list of actions needed after the consultation. If a CT scan is needed, it could check availability in appropriate hospitals and produce a list for the patient to choose from. The patient could be able to leave that consultation, whether face to face or virtual, with everything organised. There are so many more ways that technology can help. The key is in avoiding waste: wasted journeys, wasted appointments, wasted time. We are still essentially operating in a system designed for the mid-20th century. The NHS was a modern cutting-edge organisation when it was created. For me, digital health simply means us returning it to that status for the mid-21st century and beyond.
28 – Prognosis
Society of Medicine
Wimpole Street London W1G 0AE 020 7290 2900 rsm.ac.uk
Royal
1
There are so many more ways that technology can help. The key is in avoiding waste: wasted journeys, wasted appointments, wasted time.

2022
THE BIG INTERVIEW
Gene genie
Clinical geneticist Dr Melita Irving on the challenges of diagnosing and treating genetic conditions and whether genetic medicine is living up to its much-trumpeted potential
Words: Viel Richardson
Portraits: Christopher L Proctor
30 – Prognosis

w Prognosis – 31
On 20th October 2004, the Human Genome Project (HGP) published its scientific description of the human genome sequence. It was the culmination of a journey that began with the work of scientists such as Francis Crick, Rosalind Franklin and Maurice Wilkins which led to the discovery of the structure of DNA and revealed its beautiful double helix image to the world. The HGP’s announcement led to an explosion of speculation, both optimistic and dystopian, about what this might mean for humanity. Most of this interest lay in the medical possibilities the breakthrough could present. It was even suggested that by using gene manipulation we would be able to edit sickness out of humanity altogether. The reality, of course, has proved to be much more nuanced.
“That announcement was just the start of a long and difficult journey,” says Dr Melita Irving, a trustee of the Royal Society of Medicine and president of the RSM’s Medical Genetics Section from 2016 to 2019. For a start, the published DNA map only covered about 92% of the total genome sequence. It was last year, on 1st April 2022, that scientists working under the umbrella of the Telomere to Telomere (T2T) consortium finally managed to finish mapping the remaining 8%.
“The work of the HGP told us where the genes they identified were. That really opened up the world of genetic research. It was foundational to everything that has been achieved since,” Dr Irving explains. “But there is still so much we don’t know. Ninetyseven to ninety-eight per cent of the

genome is dark matter. We call it ‘junk’ DNA, but we don’t really know what it does. Within that ‘junk’ there are important regulatory regions controlling gene expression, as well as humanising elements. There is just so much more for us to find out.”
Clinical geneticists like Dr Irving focus on the genetics of disease, mainly for diagnosis but increasingly in the pursuit of cures. However, before focussing in on the genetics, they must first complete their medical training. Dr Irving qualified in paediatrics, and within that field she specialises in rare genetic disorders that affect bone development and the skeleton – a series of disorders collectively known as ‘skeletal dysplasia’. “Collaboration is a huge part of genetic medicine and I work in multispecialty, multidisciplinary clinics for patients with these conditions,” she says. “I also run clinical trials at the Evelina London Children’s Hospital researching new treatments. There are 8,000 specified ‘rare diseases’ and within that realm there are about 500 that fall under the term skeletal dysplasia.”
Dr Irving, who often comes across a lack of understanding about the nature of genetic disease inheritance, believes it is important that we find ways to educate people about both the basics and the nuances of genetic illness. “For every gene in our bodies we have two copies, one from each parent. With some genetic conditions, having one damaged copy of the gene is enough for it to develop. With others, in order for the condition to develop
32—Prognosis
What you’re looking for are those changes that are damaging – the ones that have caused the problems the patient is suffering from. You need to separate these from the harmless variations that are simply part of reproduction.
both parents have to pass on a damaged copy, meaning both copies of the gene that the child receives are faulty. This is why there can often appear to be no history of the condition in the family. The family may have been a long line of carriers, but none of them previously bore children with another carrier.”
According to Dr Irving, some of the confusion arises from the existence of genetic disorders that are not inherited but are instead caused by a change in a person’s genetic code or chromosome pattern that has occurred ‘de novo’ – out of the blue. “Not every illness that is genetic is hereditary,” she affirms.
Human genetic variation is immense. If two strangers compare their genetic code, they may turn out to be different in a million places, Dr Irving tells me. We are starting to realise that, in some respects, there is no such thing as a ‘normal’ genetic code. Some genetic disorders are caused by lots of tiny variants in the genetic code, each of which has a negligible impact on its own, but which cumulatively can lead to increased risk of things like heart disease or mental health problems. These are known as ‘polygenic conditions’. Dr Irving studies a different type of condition: problems caused by a single faulty gene.
One problem with identifying genetic conditions is the complexity of the genes themselves. If you take a blood sample from anyone, put it through a sophisticated genetic sequencing platform and examine the genetic code for changes or ‘mistakes’, you will find them. We all have them.
“In the context of clinical genetics, what you are looking for are those changes that are damaging – the ones that have caused the problems the patient is suffering from. You need to separate these from the random harmless variations that are simply part of the normal genetic code,” Dr Irving explains.
Among the many key roles our genes perform is holding and passing on the instructions for building proteins. If a gene contains faulty instructions, the proteins it produces will be faulty. Proteins are very, very important. They are found everywhere in our bodies – in tissue, bone, skin and hair. They make up the enzymes that drive many of the body’s chemical reactions as well as the haemoglobin that carries oxygen in the blood. At least 200,000 different proteins make us what we are and work constantly to keep us that way.
“If a protein is supposed to be round and a faulty gene makes it square, it can’t to do its job. That is the kind of thing that I’m looking for – a single faulty gene that is building a faulty protein that causes a problem for the patient. But even with the sophisticated tools we have at our disposal, diagnosis is still not straightforward. We continually find changes in a patient’s genes called ‘variants of unknown clinical significance’ (VUS). These are genetic variants where it’s not clear whether they’re harmful or not. You will always find VUS when you examine a patient’s DNA. As a doctor, dealing with them is a major challenge.”
Dr Irving and her colleagues use these techniques to help in this
enormous task. For example, with the rare diseases she specialises in, Dr Irving looks for rare gene variants. There are population-wide databases of genetic variants that those found in the patient can be compared against. If lots of people are known to have the variant but not the disorder, this can be ruled out as the culprit.
Bioinformaticians and clinical scientists are also able to look at a genetic variant and model the change it will make to the protein it produces. “If the structure and quality of the protein these models produce is the same as a healthy gene, we know it’s not the one we’re looking for. But if the models suggest a major change in the protein produced, that gives you a starting point for the investigation.”
A nother strategy is called ‘triobased whole-genome sequencing’. If you sequence DNA from the mother, father and child, it will show you the normal background variations in that family’s genetic code. You can look for those changes that the parents carry but which cause no issues and rule them out as suspects in the child’s condition. You can then check whether the child has any genetic changes that contrast with the parents. You can also see if both parents have a bad copy of a gene that they have passed down to their child.
T hese are just some of the strategies used to home in on the specific gene that is causing the problem. “What we do is mainly diagnostic. It involves a lot of detective work. In spite of all of the wonderful genetic sequencing platforms at our fingertips, it still requires a lot of clinical knowledge
Royal Society of Medicine
The Royal Society of Medicine (RSM) was established in 1805 with the aim of “uniting physicians and surgeons under one organisation to benefit from shared knowledge”. Originally called the Medical and Chirurgical Society of London, in 1907 it merged with 15 other specialist societies to create the RSM. Today the society’s role is to provide the highest quality education at postgraduate level and beyond to medical and healthcare professionals. It also provides a forum for discussing current medical issues in an atmosphere where innovative thinking thrives and the best ideas are disseminated. As a charity, the RSM receives no government support, thus ensuring its independence. It therefore relies primarily on membership subscriptions, support for its education programmes and philanthropy. During the Covid crisis, the RSM played a key role in providing an accessible platform for sharing clear, independent and trusted medical information. rsm.ac.uk
The Human DNA Manual: Understanding Your Genetic Code
Dr Melita Irving (Haynes Publishing, 2019)
Human Nature
Documentary telling the story of CRISPR, directed by Adam Bolt (Greenwich Entertainment, 2020)
Onasemnogene abeparvovec for the treatment of spinal muscular atrophy Hugh McMillan, Crystal Proud, Michelle Farrar, Ian Alexander, Francesco Muntoni & Laurent Servais (Expert Opinion on Biological Therapy 22:9, 2022)
w
Prognosis—33
to get to the bottom of things. We are continually sourcing clues from different areas. It’s like Sherlock Holmes trying to find the clue that nails the criminal,” Dr Irving says with a smile.
However, while diagnosis is still the geneticist’s primary function, the ability to treat some rare genetic diseases is also increasing. “The things we were able to treat first were ‘inborn errors of metabolism’. For example, there is a genetic change that means that the body can’t make enzymes that drive chemical processes the body needs to function properly. We now have treatments that allow us to cure that condition.”
Previously, if a person’s system couldn’t make an enzyme, they needed regular infusions of the missing enzyme for the rest of their life. Giving the patient gene therapy means replacing the faulty gene with one that allows the body to make the necessary enzyme. “This is where genetic engineering pipelines like CRISPR come into play,” Dr Irving says. “We can use them to create one-off treatments that offer a real cure, because the new copy of that gene will work for the rest of the person’s life. Recently there has been significant progress made with a rare neurological condition called spinal muscular atrophy (SMA) that leads to newborn babies being unable to move. They can’t even breathe because their muscles aren’t working. This is one of those conditions where you need to inherit the faulty gene from both the mother and the father. We can now put one working copy of the gene into the child and it cures the SMA.”

34—Prognosis
It still requires a lot of clinical knowledge to get to the bottom of things. We are continually sourcing clues from different areas. It’s like Sherlock Holmes trying to find the clue that nails the criminal.
The obvious question that arises is, what happens with the old gene? Will that baby still have the faulty gene and so have the potential to pass it on when they in turn have children? Is it possible that the propensity of the family to be carriers of the condition could be reduced or stopped altogether? The answer is somewhat surprising. “The propensity to passing on the faulty gene remains the same, because the new gene is not placed in your germline – the cells that make the sperm or the eggs,” Dr Irving explains. “This means that the new gene is not in a position to change the genetic instructions passed on to your children.”
But there are ways in which clinicians can hugely reduce the chances of a genetic condition being passed on when both parents are carriers. “If we take the SMA example again, you don’t know that there is a propensity to the condition in a family until they have a child who suffers from it. The way to prevent another child in the same family from having the disorder in the future is a procedure called pre-implantation genetic testing (PGT). You start with an IVF pregnancy, where you create the embryos through assisted conception. You then test them for any sign of the faulty gene and only use those embryos that are free of the condition. Using this technique pretty much guarantees that the child won’t develop the condition. The PGT procedure is reserved for severe life-threatening conditions. There are very strict rules that determine when it can be used.”
Because they involve gene manipulation in people too young to give informed consent – in this case, in babies – genetic treatments for conditions like SMA cause concerns even among clinicians. As a result, Dr Irving tells me, there are very few clinical trials currently being carried out that relate directly to genetic conditions in the very young – a situation she hopes to see change. “As a profession, our mantra is: first and foremost, do no harm. Don’t do anything that makes the patient worse – and this is even more important with children. However, a huge swathe of society is missing out on the development of treatments that clinical trials can deliver,” Dr Irving says with real feeling. “We have been running a few clinical trials in children for a number of years now, and we’ve been developing strict protocols for trials that include children.”
Generally, the earlier you start treating a condition, the better it is for the patient. As genetic conditions are present before birth, is there a point at which it would be too early to treat them? Technological challenges aside, and these are not inconsiderable, Dr Irving thinks not. “With SMA, for example, newborns can now receive treatment. But I know from research that I’ve been doing that some of the problems with the child’s bones start before birth. To me, it seems the direction of travel is to start treatment in utero, before these problems start, rather than waiting for them to develop and then trying to reverse them, which is much, much harder. But there is very little research in that area at the moment.”
Medical treatments can hardly get more controversial than manipulating the genes of pre-born children, even when it is demonstrably for their own good. It shows that, with this area of medicine, both the clinical field and the wider public are a long way from bestowing trust and confidence on genetic treatments in the same way they do with more traditional ones.
Thinking back to that initial Human Genome Project announcement in 2004, I ask Dr Irving if the world of genetic medicine is living up to its initial promise. “One hundred per cent,” she says, without hesitation. “After the human genome was published, one of the first projects was to start mapping genetic markers. Suddenly, we could see that if a person had this collection of markers they were more susceptible to inflammatory bowel disease, or if they had this other collection of markers they were more likely to get bipolar disorder. It made a huge difference in both treatment and preventative medicine. Meanwhile, single gene specialists like me started looking for single genes that might cause problems like developmental delay or the inborn errors of metabolism I mentioned. I firmly believe our main objective should be to develop new treatments for patients with rare diseases, not stop at diagnosis, which we did for so long and still do with many conditions. It has been a struggle to get where we are, but this is only the beginning. The possibilities that genetic research has are enormous and I think it is our duty to discover and develop them.”
Prognosis—35
BEYOND THE PITCH

36 –
Prognosis
Dr Jesus Olmo of Isokinetic is renowned for his successful stint as medical director at Real Madrid. He talks about the knowledge and experience he brought from the world of elite football to offer the clinic’s patients
Words: James Rampton

w Prognosis – 37
Most eminent doctors have impressive medical certificates on their walls. Not Dr Jesus Olmo.
The wall of his office at the Isokinetic Medical Group on Harley Street is decorated with a white Real Madrid shirt, three replica Champions League trophies and two FIFA World Club Championship gold medals. The display is testament to the role Dr Olmo and his team played in one of the club’s most successful periods.
In September, Dr Olmo joined Isokinetic, one of the leading specialist sports medicine and rehabilitation groups in the world, as a consultant in sports orthopaedics and rehabilitation. Prior to that, between 2013 and 2017, he was medical director at Real Madrid, where he worked with some of the very best football players on the planet.

Speaking from his office at Isokinetic, Dr Olmo tells me he really enjoyed dealing with these elite players. He was particularly impressed by the Welsh star Gareth Bale, who recently captained his country in the World Cup. A doctor blessed with an engaging bedside manner, he says: “Everybody knows that Gareth is an absolutely amazing player. In terms of technical quality, he is one of the most talented players I’ve ever seen. He is an outstanding football player, but he could also have been a good rugby player, a good athlete, a good tennis player, or whatever he wanted to be. He is a major natural talent.”
Dr Olmo’s principal achievement at Real Madrid, however, was not helping some of the best players on earth, but revolutionising the way the medical department at the top Spanish club was run. To borrow some football cliches, he transformed Real Madrid’s medical services from an old-fashioned ‘route one’ method of treatment to a supersophisticated, cutting-edge, ‘tiki-taka’ system.
According to Dr Olmo, who is also the director of The Doctor Olmo Clinic in Granada, Spain and co-founder of the Football Science Institute FSI, “people think of Real Madrid as a very successful team, but when I arrived at the club in 2013, that was not the case. We had been beaten by Barcelona for many years and had not won the Champions League for 12 years.”
Dr Olmo immediately realised that changes had to be made – and fast. That is far easier said than done, though, at an institution as conservative as a football club. The 56-year-old doctor, who from 1995 to 2000 was the head of medical services for the Spanish Rugby Union, explains. “Football clubs can be very traditional. They think that they are perfect and that things should be done in a certain way because they have always been done that way. So when you come from another sport – in my case, rugby – and you want to do things differently, they say: ‘No, no, that won’t work. This is football.’ You know it’s going to be difficult, but you have to stick to your guns.”
So Dr Olmo dug in his heels and set about dismantling the traditional structure of the club. He confesses that to begin with, “it was pretty controversial”. He had to engage in a diplomatic game. “There are different interests at play. People think that the club, the coach and the players all have the same interests, but that’s not the case. It’s very difficult to make everybody happy.”
But that did not stop Dr Olmo. “We changed many things, but the main thing was that I acted not only as head of medical services, but also head of performance. So I was not only taking care of the injuries, but also helping to prevent injuries, to treat chronic injuries, and to manage the load, the recovery and nutrition performance
38—Prognosis
Above: Dr Jesus Olmo
for every player individually.”
Dr Olmo also regularly checked in on the club’s most valuable assets: the players. They are all individual, highly successful businesses, generating millions of dollars and employing dozens of people, so their general welfare is vital.
Unlike players of the past, who used to train on a diet of pies and pints, the sportsmen of today have highly advanced training regimes, which they follow to the letter at home. Extremely disciplined, they all pay a great deal of attention to detail and display a champion’s attitude to fitness. The doctor’s job is to ensure that they are content and able to focus on their training.

Dr Olmo asserts that, while most players have to adopt a tough or arrogant image to hold on to their place in a very competitive environment, in private the majority of them are charming. At Real Madrid, he recalls, “I had a lot of autonomy. I developed a very good relationship with many players. I went to their homes because I understood it was my duty. I was hired by the club to take care of the players, and I couldn’t do that if they didn’t have confidence in me. I needed to show them I was there to help them.”
In the end, Dr Olmo’s persistence paid off. Those at the club who had been dubious about the radical changes he brought in were ultimately won over. “Individual high performance is good for everyone,” he says. “No matter what sport it is, it is a question of analysing every aspect of the athlete to do with performance and trying to improve it incrementally with what we call marginal gains. Those little improvements can make a big difference. It’s the future. And fortunately, at Real Madrid, it worked.”
Once the club started winning the Champions League,
w Prognosis—39
I developed a very good relationship with many players. I went to their homes because I understood it was my duty. I was hired by the club to take care of the players, and I couldn’t do that if they didn’t have confidence in me.
people conveniently forgot their complaints about Dr Olmo’s changes. The experience taught the consultant a great deal about diplomatically overturning tradition, about breaking new ground tactfully, both on and off the pitch.
Now Dr Olmo is bringing his years of expertise from Real Madrid to Isokinetic, which is recognised as a FIFA Medical Centre of Excellence and treats a very large number of high-level sportsmen and women as well as non-athletes who have suffered an injury. The consultant is part of a major drive at Isokinetic to revolutionise the field of sports science.
One of the most significant ideas that he is transferring from the football club is the holistic philosophy of medicine. He outlines what that means: “We are looking at the whole person. At Isokinetic, the goal is not just healing a knee injury; it’s bringing the patient to their desired level of performance. Obviously, to bring the patient to this level, you need to heal the injury, but also take care of why this knee injury has happened because maybe there was something wrong before it occurred.


“So the whole body and mind come into play. We take care of every single aspect that can influence the physical conditioning and the performance and the health of the patient. For me, health and performance are the same thing. They are good for each other. Performance without health is not possible.”
Dr Olmo, who also oversees trailblazing work in GPS monitoring and platelet-rich plasma (PRP) injections at Isokinetic, also firmly believes in the importance of communication between doctor and patient. “You must detect how the person you are talking to is feeling. That helps
to shape your language with them. Medicine is an art, and it has a lot to do with confidence and trust. A doctor should communicate with a patient not only to have a clear diagnosis or good analysis, but to develop trust. It’s about discovering how you inspire confidence in the patient because that’s also good for healing.”
These encounters, he adds, “teach you how to manage top athletes, how to talk to them, how to understand their interests and in the end how to encourage them to have the best possible treatment.”
40—Prognosis
When a football player who we know is prone to certain injuries comes to Isokinetic, we can detect things about them that can’t be detected in other settings.
Far left: The Green Room at Isokinetic Left: On-field rehabilitation in Regent’s Park Opposite: The Isokinetic clinic on Harley Street
The area of injury prevention is also absolutely central to the work Dr Olmo is performing at Isokinetic, which has been a pioneering force in sports medicine since its foundation in Italy in 1987. A club will inevitably perform far better if it is able to field the same team every week. Look at the table-topping, pre-Christmas performance of Arsenal, who were able to put out virtually the same 11 for every game.
“We know a lot more about injury prevention than we did 10 years ago,” says Dr Olmo. “Injury prevention is not an easy thing. It is not just doing a couple of exercises. You have to assess the player’s individual body – how it’s built, its genetics, the alignment of the lower limbs. Does it have a problem controlling those limbs, has it developed muscle imbalance or joint stiffness? We can check many things about the individual player’s predisposition. But then, they must go through a training process that’s about managing load, recovery, rest, nutrition.”
One of the other innovations at Isokinetic, whose 200plus staff see thousands of patients every year, is the Green Room. This has nothing to do with the theatre – rather, it is a crucial advance in sports rehabilitation. “It’s called the Green Room because the floor is green like grass. It is a room with a force platform, lots of cameras and a big screen in front of the patient. The patients can see themselves performing all the things connected to their athletic activity – landings, changing direction, lateral strides, accelerations, jumps.
“Imagine that you are a tennis player. You need to go to the ball and strike it with energy on one side and then go to the other side and do the same thing. We can retrain that player very easily in the Green Room setting. Because we have cameras and the force platform, we can measure how the
patient controls their lower limbs. That is a big advantage because sometimes the patient says, ‘OK, I have recovered my strength, I feel well.’ But we can measure his readings to be sure he is able to control the movements in his lower limbs, so he is performing well and with a low degree of injury risk. So it’s a massive tool for us.”
While any clinic could more or less replicate the set-up, it’s the knowledge behind all the thousands of evaluations that makes the Green Room unique. Isokinetic is sitting on a gold mine of data. That’s why, for example, “when a football player who we know is prone to certain injuries comes to Isokinetic, we can detect things about them that can’t be detected in other settings. That way, we can provide the means to correct deficiencies.”
I ask Dr Olmo what prompted him to leave professional football for Isokinetic. “I am a sports medicine and rehabilitation doctor. For me, Isokinetic is the best sports rehabilitation organisation in the world. The methodology developed here is much more advanced than at any football club. The work I do here is very rewarding as well. We have a huge number of patients most of whom are not professional athletes who come to our parties and our meetings. They’re part of our family. They are so happy and grateful to us. That enduring feeling of gratitude is one thing I love about this job. Isokinetic really is the summit.”

Prognosis—41
Isokinetic 11 Harley Street London W1G 9PF 020 7486 5733 isokinetic.com

42—Prognosis
T TIME
CAR-T therapy, a form of cellular immunotherapy, offers huge promise in the treatment of cancers. Doctor Mike Potter of The Royal Marsden explains how it works and why it holds so much promise
Words: Gerard Gilbert
Portrait: Dominick Tyler
w Prognosis—43
“It is the perfect targeted cancer therapy,” says Doctor Mike Potter, consultant haematologist at The Royal Marsden. We are discussing CAR-T therapy, a promising form of cellular immunotherapy that Doctor Potter and his team have been using for the past three years on lymphoid cancers such as non-Hodgkin lymphoma.
P ut simply, CAR-T therapy modifies patients’ cells so that their immune system’s natural ‘attack dogs’, the T cells, start to go after tumours in the same way that they already fight infections. Chimeric antigen receptors (CAR) are introduced to the patient’s T cells, which are then able to recognise and latch onto the tumour cell and destroy it.
“A CAR-T cell is a T lymphocyte that’s directed against malignant cells,” explains Doctor Potter. “CAR-T cells are infused into the blood and because they’re lymphocytes – a type of white blood cell found in the immune system –they flow around the blood system and lymph glands, so they’re already in the areas where you want them.”
Patients deemed ready for the treatment have their blood samples sent off to a pharmaceutical laboratory in the United States, as Europe is still in the process of building its own processing labs. It takes two to four weeks to extract and modify the cells before they are returned to The Royal Marsden and infused back into the patient.
“It’s best to collect these cells before you give lots of toxic chemotherapy because that will reduce the yield of the cells and make it less effective,” says Doctor Potter. “We’re treating
mainly lymphomas, B-cell lymphomas, which are 90% of all the non-Hodgkin lymphomas, and acute lymphoid leukaemias (ALLs) in children and young adults.”
Blood malignancies respond well to the therapy because CAR-T cells travel around the circulatory system. “The licensed therapies involving CAR -T cells in the UK are restricted to non-Hodgkin lymphoma and acute lymphoblastic leukaemia, so lymphoid disorders,” Doctor Potter explains. “CAR-Ts seem to work better for lymphoid disorders than myeloid disorders”
The former are the cells of the immune system that fight infection, while myeloid diseases come from myeloid precursor cells, usually in the bone marrow. “And that’s a different type of cell fight,” adds Doctor Potter.
On the question of whether or not CAR-T might be used against solid tumours, the likes of lung, breast and prostate cancer, the doctor is guardedly hopeful. “There are no licensed CAR-T therapies for the solid tumours that are not haematological [blood based] at the moment,” he says. “But there are already clinical trials underway on certain solid tumours. The challenges are different.
“For some cancers it looks promising. There’re some protocols in brain cancer, where instead of infusing it into the blood, they infuse it into the fluids around the brain. But mainly it’s for tumours where there’s an immune element of controllability – like renal cancer and melanoma. These are tumours that have been amenable to further immunological approaches.”
CAR-T, which is available both
privately and on the NHS, is an expensive treatment at the moment, but it is hoped that, as with other treatments, it is hoped that the cost will eventually start to fall. “The expense relates to all the research and development that the drug companies have had to do in making this technique of introducing proteins on the lymphocyte surface through a gene therapy protocol,” says Doctor Potter. “Issues of safety, quality control and efficacy all have to be thoroughly investigated.”
A fall in the price of the procedure will allow the treatment to be more widely used. At the moment, it is targeting an extremely ill group of patients. It is generally used for people who’ve failed two lines of conventional treatment – such as chemotherapy and stemcell transplant. They also need to be resistant or relapsed after the standard treatments.

“Basically, it can cure some otherwise incurable cancers,” says Doctor Potter. “It’s not an option for first-line treatment. But it’s there after the failure of first-line treatment and as an option for second-line or beyond. It’s targeting a very vulnerable group of patients who would otherwise probably not survive. And the results have shown a high response rate with about 30-50% of patients doing very well long term and hopefully cured.”
He feels that should CAR-T therapy become a first-line treatment, perhaps one day supplanting chemotherapy, the advantages would be enormous.
“It’s immunology, so it’s harnessing the power of the immune system to
44—Prognosis
Chemotherapy can only be given for a limited period, so either you cure the cancer or it comes back. CAR-T therapy offers a continued immune surveillance against the tumour returning.
kill off the cells,” says Doctor Potter. “Chemotherapy is extremely toxic to your normal tissues as well as the tumour cells. It can also only be given for a limited period, so either you cure the cancer or it comes back. CAR-T therapy, on the other hand, is an ongoing treatment because the CAR-T cells persist. It’s a continued immune surveillance against the tumour returning.
“We hope that with that first treatment you’ve got a long and durable exposure to the benefits of immunotherapy. Because cells continue living and growing inside the patient, one assumes that if the tumour showed signs of coming back, then the cells will respond to that and go and mop it up.”

Not that chemotherapy would be replaced entirely by CAR-T as it is used in the lead-up to infusing the modified cells. The patient needs to go through three days of chemotherapy, which is immune-suppressive, to allow maximum expansion of the infused CAR-Ts. The aim is to take away a lot of the competitor cells, so when these CAR-T cells come in, they can grow and expand quickly.
A lmost inevitably there can be some side effects from CAR-T, the most common being cytokine release syndrome (CRS), which can occur within 24 hours of the infusion. The massive expansion of lymphocytes in the system releases a lot of chemicals that help fight against infection and the tumour cells.
“The patients may have a fever, have problems with their blood pressure falling, may become oxygen-dependent, feel very unwell, and that’s cytokine release syndrome,” says Doctor Potter.
w Prognosis—45
CAR-T therapy can cure some otherwise incurable cancers. It is targeting a group of patients who would otherwise probably not survive.
Above: Doctor Mike Potter
“It can be very mild or it can be lifethreateningly severe and mean the patient being transferred to intensive care for monitoring and treatment.”
Another potential side effect is neurological toxicity. “That’s less understood, but I think it relates to the chemicals and a leaky blood-brain barrier and some sort of toxicity of the cytokines within the brain,” he says. “Patients can become confused, have memory problems and difficulty moving their arms and legs. They can also have fits, and they can become unconscious in very severe cases. That’s an unusual toxicity with chemotherapy but we see it with these immune therapy protocols.
“ The good news is that we can control those complications. In nearly every case they are reversible. But you need to be in hospital and you need powerful drugs to treat it. We haven’t lost a single patient – out of around 40 to 50 – from these complications, so the patient mortality has been zero. Not all the patients are cured, but a high proportion have had a good response and they’re doing well in what is still a relatively short follow-up period.”
The CAR-T cells have two distinct parts, each with a different task. The outside of the receptor is the CD19 antibody: this recognises and latches onto the CD19 protein, attaching the T cell to the tumour cell. The other part is inside the CAR-T cell, and this sends a signal for it to activate and kill the tumour cell. The secondgeneration CAR cells, currently in use at The Royal Marsden, have a ‘co-stimulation’ modification – the
part that sends the signal to activate the CAR-T cell.
“So, it’s stimulating the T cells to become more active,” says Doctor Potter of this modification. “The third generation of CAR-Ts looked at a double dose of stimulating molecule and then the fourth generation are looking at additional constructs that are artificially introduced that release more of these cytokines locally to the tumour cell. It’s getting really complicated but basically, we’re ramping up the power.
“Another thing that’s being developed are dual-CAR-Ts which can each target two proteins. Within lymphomas that could be the usual target, which is known as CD19 and then another one such as CD20. Doing this increases the chance that you get maximum cell kill.”
There’s little reason for me to ask Doctor Potter how excited he is about the future prospects for the therapy because he manages to more than adequately convey his enthusiasm in his tone of voice. “The field is potentially huge because we know that the technology works,” he says. “People were worried about introducing a genetically modified protein receptor but there seem to be no side effects from that in terms of ‘can it activate other genes that cause cancer?’ We haven’t seen any evidence of that.
“ The genius of it is that the T cells expand in the processing in the lab and then they expand in the patient. These are all genetically modified, they’re all going to have that receptor for the tumour and they’re going to go in there and smash it to pieces. And we’ve got scans of
patients with large tumour masses that have not responded to chemotherapy or radiotherapy – two to three weeks after CAR-T, it has completely disappeared. It’s unbelievable.
“In some patients, these CAR-Ts persist for years and that correlates to long-term disease survival and cure. Sadly, in some the CAR-Ts decay and decline and disappear. There’s the risk of relapse in that situation. Why does that happen? We’re not quite sure. We’re at the beginning of the learning exercise – just five years into it. Allogeneic transplants using stem cells as part of cancer treatments have been around for 50 years and we have made huge progress. With medical advances happening at an increasingly rapid pace, who knows what we will be capable in the next 50 years?”
46—Prognosis
The
19a Cavendish Square London W1G 0PL 020 7811 8111 royalmarsden.nhs.uk
Royal Marsden Private Care at Cavendish Square
We’re at the beginning of the learning exercise – just five years into it. With medical advances happening at a rapid pace, who knows what we will be capable in the next 50 years?
THE HARLEY STREET BUSINESS IMPROVEMENT DISTRICT
The Harley Street BID has been established to promote the area and represent the exciting mix of businesses here. In November 2021 the business community were invited to vote in the ballot to develop a business improvement district and there was an overwhelming “yes” for a BID to be established from the businesses. The BID term runs from April 2022 to March 2027. With the investment that will be made through the BID this provides opportunities to deliver projects across the key themes which are set out below.

STRATEGIC THEMES
Our next steps involve identification and project delivery, looking at key priorities and setting our steering groups with key partners. Our 4 steering groups are set out below and we will have a specific medical group to ensure we acknowledge and deliver opportunities for all businesses.
If you would like more information on the newly developed business improvement district please do not hesitate to contact Nicki Palmer. Email: nicki@harleystreetbid.com Telephone: 07944 386903
GET IN TOUCH
Follow us on social media: @Harleystreetbid Harley Street Business Improvement District www.harleystreetbid.com PUBLIC REALM AND WAYFINDING INTERNATIONAL MARKETING BUSINESS SUSTAINABILITY AND CONNECTIVITY SAFETY AND BUSINESS RESILIENCE
Q+A
Female pelvic floor issues
Alexander Bader of the Bader Medical Institute of London on pelvic floor issues and why women shouldn’t suffer in silence
Words: Viel Richardson
Portrait:
Christopher L Proctor
What is the pelvic floor?
The pelvis is a basin-shaped structure which supports the spinal column and protects the abdominal organs. The pelvic floor is a complex series of muscles and connective tissue in the pelvic area that has two main functions. One is to provide support and protection to the organs in the area. In the case of women, it protects the uterus and ovaries, as well as the bladder, bowel and rectum. The other function is to keep the continence mechanisms working properly. Both sexes have a pelvic floor, but we deal exclusively with female pelvic floor issues at the clinic.
The pelvic floor can be too loose or too tight. What causes these situations to develop?
The more common issue is a loose pelvic floor, where the muscles have lost their condition, been damaged or become stretched. This can happen through traumatic injury or though some of the normal functions of a woman’s everyday life. It may be the result of an invasive delivery, where there has been an issue during the birth of a child, but sometimes a normal delivery can cause some damage.
A patient losing a significant amount of weight quickly can cause a pelvic floor collapse. Patients suffering from a long-term chronic cough which constantly puts pressure on the lower abdominal wall can develop muscle looseness. Also, patients who drink or smoke heavily have an increased risk.
What symptoms will pelvic floor looseness cause?
The first is urine incontinence where the patient is unable to control or hold their urine. When they cough, sneeze, exercise or do other daily activities they can leak a small or significant amount of urine. The other major issue is organ prolapse, where an organ falls or is forced out of its proper position. For example, patients could suffer a rectocele prolapse which is a prolapse of the rectum, a cystocele prolapse which involves the bladder, or a uterine prolapse where the uterus slips into the vaginal canal, sometimes protruding out past the cervix. As you can imagine these can be very uncomfortable and distressing. They can also cause multiple and recurrent infections, putting the patient at risk of more serious illness.
What about pelvic floor tightness?
This is far less common and almost always a secondary symptom caused by a separate problem. Unfortunately, it is often the result of poor corrective surgery – at our clinic around 2025% of our patients are coming to correct complications caused by previous surgeries. Possibly a woman encountered difficulties during delivery, meaning that afterwards the surgeon placed some stitches in the pelvic floor or the vaginal canal, which were done incorrectly. Primary pelvic floor tightness might be caused by an anatomical deformation that someone was born with, or by physical or psychological trauma. In the last case you are looking at a very different treatment path.
48—Prognosis
Mr

w Prognosis—49
What are the symptoms here?
The impact is more severe for the patient as these women are not able to have sexual intercourse. This can be catastrophic for a couple, particularly one that wants to start a family or have more children. With tightness, the severity doesn’t matter – the woman will always suffer from significant pain. The muscles and other tissue can be stretched, distorted and can develop fibrosis, which is excessive accumulation of fibrous connective tissue. The patient won’t have suffered from incontinence, but the pain can make other everyday functions difficult.
How do you characterise the seriousness of a pelvic floor issue?
We characterise the situation in three stages: mild, moderate or severe. The determining factor is the seriousness of the impact on the woman’s life. Pelvic floor issues are not fatal, but left untreated they can have a disastrous impact on the patient’s quality of life and mental health. When it’s mild, we can treat the situation in minimally invasive ways, but with a moderate or severe diagnosis you are looking at a surgical intervention.
What are the different treatments available to you?
It is key not just to classify the severity but also to understand where the patient is in her life’s journey. For example, if she is looking to have more children, we rule out surgical treatments. With mild cases we start with Kegel exercises, which target and strengthen the pelvic floor muscles.
The problem is that these can be tricky to do correctly at home. At the clinic, we have a specially designed chair, the EMSELLA chair, which can produce 11,000 contractions of the pelvic floor muscle within half an hour. It requires very little effort from the patient, is pain free and targets the muscles correctly, so is very effective. After this we might move on to laser treatment or radiofrequency. Other treatments available are biological treatments such as using the body’s own stem cells, growth factors and exosomes –which are central to communication between the cells. The aim is to improve the quality of the tissue and strengthen the muscles.
What about when symptoms are more severe?
We may have no solution other than surgery. This might involve correcting the anatomy if organs are in the wrong position, repairing things that have been damaged, or working to improve the quality of the tissue in the area. As a surgeon, your primary aim is to restore the best possible function. There are occasions where the patient says that everything is now working, but aesthetically she’s not happy. Improving the appearance is possible once the body has completely healed from the initial surgery, but our primary goal is always to correct the function, to make sure that everything is working well and positioned as close as possible to where it should be.
Are pelvic floor procedures difficult?
All surgery is difficult because you’re
dealing with a living human body. But yes, pelvic floor procedures can be complex and difficult. The area contains several sensitive organs, muscles and connective tissues, all in very close proximity. There is a risk you might correct one organ but damage another. However, in the hands of a skilled surgeon who is experienced in such work, it should be fine.
Are there patients who are not suitable for pelvic floor surgery?
I would advise strongly against any kind of surgical intervention for a woman planning to have children, because giving birth would destroy whatever correction the surgeon has done. Not only that, the damage would be more severe because of the previous surgery. If a patient is suffering from vaginal dryness, we need to correct that in parallel to or even before any surgical intervention. Also, very obese patients are not really suitable and if a patient has a chronic long-term cough you need to address that before moving forward.
Aside from traumatic causes, is a particular demographic more likely to have pelvic floor issues?
Statistics shows that the number of people suffering from prolapse, incontinence and pelvic floor looseness increases with age and is much higher in women over the age of 80. However, that number is moving in the wrong direction. In our clinic we are treating an increasing number of people in their fifties and even forties. I believe this trend is related to lifestyle. Many patients are not well exercised, are
50—Prognosis
overweight and are heavy smokers or drinkers, all of which increase your risk of developing pelvic floor issues.
What usually brings patients to the clinic?
Often, it is some level of organ prolapse, ranging from mild where things just don’t feel right to severe where an organ is protruding. After that, it’s incontinence. Unfortunately, incontinence can be a taboo subject. There is this idea that it comes naturally with age and that women just have to live with it. We are doing our best to inform them that they do not have to keep suffering, as there are ways we can help. We also get
patients who come seeking aesthetic improvements.
Are there some issues that should be dealt with quickly?
In cases of severe prolapse where the organs are protruding, or severe incontinence where the patient has little or no control over urination, I need to deal with this very fast. If a patient arrives with an over-tightened pelvic floor or vaginal canal and is not able to have any kind of normal sexual intercourse, it needs to dealt with immediately because this is a lifechanging condition. None of these will kill the patients if left untreated, but they bring an increased risk of other
infections and the impacts on their life and mental health can be very serious.
Is addressing the mental health side something you do?
We think it is very important to do so. Alongside the clinical psychology department at Oxford University, we are developing questionnaires that help to detect patients who may be struggling as a result of pelvic floor issues. There will be questionnaires for both the clinicians and patients. The idea is to detect at-risk patients early so we can intervene in the appropriate way. Also, we want to follow people after a surgical correction to see how they are doing. At the moment, we are running a clinical study which will be published next year. Questionnaires will then be available to all professionals involved in this field.
What do you like most about your job?
I love my job. In training I saw many issues where the response from older surgeons was that this was entirely natural and there was nothing to be done. I thought, no. I know the anatomy and have the surgical skills, I want to see what I can to to help. When I see patients who arrive in pain and distress coming back to my clinic, smiling, laughing, living a full life, it brings me great satisfaction.
Bader Medical Institute of London 75 Harley Street London W1G 8QL 020 3149 9147
badermedical.com
Prognosis—51
Pelvic floor issues are not fatal, but left untreated they can have a disastrous impact on the patient’s quality of life and mental health. When it’s mild, we can treat the situation in minimally invasive ways, but with a moderate or severe diagnosis you are looking at a surgical intervention.
52—Prognosis
Miles Eckersley on how Mako robotic hip surgery got him back on his feet
I’d probably needed a new hip for a good five years, but I’d just let it run. One reason for the delay was that I’d had private medical insurance but then moved jobs. The new insurers had a moratorium on pre-existing issues, which meant I had to wait two years before I was covered again. Eventually the day came that I could ring the hospital and say: “I really need to get this done now!”
By then, the pain was really affecting my life. I couldn’t sleep. In that last year, it was awful. If I walked more than a mile or so in the morning, I was out for the afternoon because I simply couldn’t move. When the pain first began, I had no idea it was to do with my hips. I had really bad back pain, so I went to see a physio. I’m not usually someone who’s very good at going to physios or doctors, but this was so bad I was going daily. Three or four days into the physio sessions, the physiotherapist told me that this wasn’t about the back at all and referred me to have an MRI scan.
The scan showed that I had bad wear and tear around my left hip. It was almost bone on bone. I kept thinking, I must get that booked in for treatment, but of course work takes over and you put it off because you’re busy. I didn’t get it done for a couple of years, then I moved jobs and had to wait two more years for the insurance to kick in.
I had terrible cramps down my legs. I had to sleep with a pillow to hold my left leg away from my right leg, because if they came together it caused excruciating pain. If I did any kind of exercise, I could push through the pain barrier, but afterwards it would be extremely painful – shooting pains
down my leg and up my back. Gradually I found I couldn’t bend over to pick things up. I have got a very high pain threshold, so I just got on with it.
A physio in Richmond had recommended Mr Simon Bridle and said he was doing this Mako robotic hip surgery. She called him on my behalf, and I quickly heard back from his secretary, Adriana, who was lovely. She emailed me and said that Simon would see me the next Thursday. I’d been to see another consultant previously and he’d forwarded the x-rays and scans.
Simon told me that I had bad wear on the right hip as well as the left and that it would be best if we did them both together. Hearing that, I felt quite elated but also shocked. That was early June 2022, and he said he could fit me in at the end of June, just weeks away. I was thinking, “Oh my God, this is real happening!” I was quite concerned about the operation length and the effect the drugs could have on my heart, but he told me not to worry about it. We’d do the left one first and if we had to stop, we could always do the right one another time. I thought that sounded reasonable. I did jokingly ask if, as he was doing both at the same time, he could maybe add an inch on each leg to make me a bit taller, but alas he couldn’t!
Adriana organised a visit to the Cromwell Hospital for the pre-op, which was all very straightforward, and then I had another MRI scan. I must admit, I was still quite nervous about the operation. I’ve had a few ops before – a hernia and a snapped achilles – but this felt like quite a big one. But in the end, it was all very straightforward.
Simon did both hips at the same time and there was no problem. After I came round, I couldn’t have even told you what day it was, but apparently I spoke to my sister at length. She said she’d never heard me chat so much.
I was only in hospital for three days. I was able to walk the day after my operation. I walked to end of the corridor and back, and it was amazing. You’ve got to be careful not to push yourself, though.
I didn’t have much post-operative pain at all, really – I didn’t need to take many of the painkillers. I’m still a bit numb on the tops of my thighs and the sides of my buttocks. I occasionally get short bits of fiery pain in my legs, but it’s a very different sort of pain, and nothing like what it was. Simon told me it takes 12 months to fully recover and I’m only five months in.
I’ve got four scars – two large ones, which are about six inches long on each leg, and then just above that on either side there are two smaller ones about an inch long where they bolt the robot just above your hip bone.
My lifestyle is gradually changing since the operation. I climbed a mountain in September, just three months after the op. I had sticks to help me. It was 800m up to the plateau, down again and around the lake –about 8-9km in all. I used to cycle with my legs sticking out like Joey the Clown because I couldn’t bring my legs together parallel, but now I can cycle normally. I used to do a lot of rowing on a rowing machine, but I had to do it with my legs out – I can now do that properly too.
w
Patient experience
Prognosis—53
Osteoarthritis A condition in which the cartilage which – a firm, slippery tissue that enables almost frictionless joint motion – deteriorates. This causes stiffness and pain in the joint.
Echocardiogram (ECG) A recording of the heart’s electrical activity which enables clinicians to check the performance of the heart.
Intraoperative A usually unplanned or associated procedure or correction that can be performed during the course of a larger operation.
WHAT IS MAKO ROBOTIC HIP REPLACEMENT?
Mr Simon Bridle, consultant hip and knee surgeon, Fortius Clinic
It’s often the little things that suddenly make you realise what a change it has made. The other day I got down on my knees to clean the fireplace. Things you take for granted – like just getting up from the sofa –were really difficult, and now I can do them again. My wife said I used to walk like an old man and now I’m standing taller, my posture’s better. Before, at weekends, if I took the dog for a walk for an hour I’d be knocked out for the rest of the day. But now if my wife says, let’s jump on the tube and go into London, we’re able to go.
I really love skiing. All my family ski. Last March was the last time we went and I couldn’t do it properly. I had a really bad fall. I wanted to go one way and my hips wouldn’t allow it and I ended up head-planting in a nasty way. It was quite devastating at the time. We were supposed to be going out that evening and I couldn’t move; I had to be helped into the car like an old man because I’d fallen over so badly. Mentally I felt massively down. I’m still not allowed to ski, but even just pretending to ski, making those skiing movements, I can now bring my knees together, which I couldn’t do before. I’ve got March as my goal to strengthen my legs to go skiing with the kids.
Without a doubt, I’d recommend the surgery to anyone. As long as you can get over that initial shock of having both hips done at the same time, it’s for the better because ultimately your recovery time is quicker. With the robotics, there’s less chance of one leg ending up longer than the other. I’d say, don’t procrastinate. It’s given me a new lease of life.
Osteoarthritis is still a very ill-understood condition. We don’t really know what causes it. It’s simplistically called ‘wear and tear’, but it is basically when the lining cartilage just goes away and you end up with bone rubbing on bone. The joint forms extra bone called osteophytes (bone spurs) which grow around the joint and cause stiffness and pain. This reduces movement and mobility and has a profoundly degenerative impact upon quality of life.
The pain affects everything from day-to-day tasks and activities to sleep and general physical and mental health. If left untreated it can lead people to becoming increasingly disabled. Hip arthritis is unbelievably common and there are around 100,000 hip replacements performed each year in the UK.
In Miles’s case, while he came to see me for his left hip, it was clear to me straight away that his right hip was also in a state of significant decline. When both hips have deteriorated to this extent, a double hip operation can mean a speedier recovery time overall, and reduced risk, as it only requires one surgical procedure. The Mako robotic hip replacement procedure adds a further layer of benefit as it improves the accuracy of the replacement.
One of the biggest problems with traditional hip replacements is that you can end up making the leg the wrong length. Using robotic surgery allows you to almost guarantee the leg length is always right. It has other benefits too: dislocation is where the ball and socket come apart, and this is incredibly painful, but putting the parts
in more accurately minimises the risk of dislocation. We are also able to better reproduce the patient’s own anatomy. The relationship between the femur and the pelvis is very important in terms of how the muscles around it work and can differ from person to person.
Every patient having a hip replacement has a pre-assessment where they come to the hospital to have blood tests done, have an ECG, have their general health checked over. At the same time as you do the pre-assessment you have the CT scan, which is usually needed about two weeks before the operation. The scan is sent off to the US, which is where the robotics centre is located, and they do the plan and send it back to the surgeon to be adjusted accordingly.
You have to teach the robot where the patient is in the operating room by putting a reflecting array, which is three reflecting balls, in pins into the bone. There’s a camera which sits in the operating theatre and can see the reflecting array. You then do “registration”, which is to select a number of different points on the bone and thereby teach the computer where the bone is.
The robot doesn’t carry out the operation – it acts as a passive assistant to the surgeon, helping you ensure the accuracy of implantation. Once done, you can adjust things intraoperatively within 1-2mm.
Fortius Clinic
17 Fitzhardinge Street
London W1H 6EQ 020 3195 2442
fortiusclinic.com
54—Prognosis
arthritic
An
hip Diseased cartilage
Mako
robot A replacement hip
Hip implant Pelvic bone
Prognosis—55
Femur (thigh bone)

56—Prognosis
SERVICE SECTOR
Lina Patel, associate director of cancer services at The London Clinic, on the importance of combining clinical innovation with holistic care
Words: Gerard Gilbert

w Prognosis—57
“Cancer treatment is a fast-paced, dynamic, innovative agenda – there’s always something new and I’m really passionate about what I do here,” says Lina Patel, associate director of cancer services at The London Clinic. “Not just the clinical innovations, but the holistic nature in which the patients are looked after.”
Patel, who has been working in cancer services – mostly private, but also within the NHS – for more than 35 years, is discussing the clinic’s new ‘one-stop’ service. While the term ‘one stop’ gets across an important part of the new offering, she is keen to stress that this description only applies to the diagnostic element. Once the diagnosis has been made, the new service also incorporates first-rate treatment and support services, which involve precisely as many ‘stops’ as the individual patient requires.
“I just want to be sure that we understand that ‘one stop’ means that if a patient has got a suspicious lump, or an area that could have cancers, we do all the tests and consultation on the day and the patient will get the results within the 48 hours,” she explains. “To be honest I think it should be called ‘rapid expert diagnostics’, because it’s streamlined in such a way that patients have access to knowledge about whether they’ve got cancer very quickly.”
Such a rapid diagnosis obviously negates a lot of the worry and uncertainty caused by waiting, often for weeks on end and especially given the delays in cancer treatment caused by the Covid backlog. So, how would the patient experience such a ‘rapid expert diagnosis’, from the moment they walk through the doors of The London Clinic to the moment they receive their diagnosis?
“A planned appointment will have been made in advance so they wouldn’t be waiting for four or five hours after they
arrive,” says Patel. “We expect them to be seen within the hour and all the other tests would be booked for them and aligned. Typically, a patient would spend maybe two, or two and a half hours, altogether. We have designed a package for fast-track rapid access so the patient will know exactly what it will cost them in advance so there are no surprises.”
Tests for breast cancer include a mammogram and an ultrasound, and during the latter examination the doctor will also take a biopsy. “And then they will go home and we’ll give them the final result of the biopsy within 48 hours. The diagnosis is accurate because we’re using the top end of the tech with the mammogram and ultrasound, and we’ve got radiologists who are specialists in reading those.”
If and when cancer is diagnosed, the consultant will tell the patient and then go through the next steps with them. Further tests will pinpoint what stage the cancer is at, whether it’s been caught early or spread further. The patient will then be assigned a named nurse specialist who will be their key worker and will be able to answer any questions and keep them informed about further tests or treatments.
“We’ve got a multi-disciplinary team – other surgeons, radiologists, pathologists – to finalise the recommendation for treatment,” says Patel. “They look at the images and the pathology and then make a joint decision about the treatment so that the consultant can go back to the patient and present the options. The patient will be given some time to make their decision – it is important that they feel they are making an informed decision. But unlike the NHS at the moment, we are in a position to start the treatment very quickly.”
The clinic provides several cutting-edge forms of treatment, Patel explains. “We’re in the process of replacing our linear accelerators which deliver radiotherapy, and
58—Prognosis
we’ve invested in the latest radiation therapy machine. One of the other new things we’re doing is CAR-T therapy for haematological cancers and that will expand to other conditions as the treatments become available in the UK. Cancer care is transforming at a great pace, and we are able to offer targeted treatment using immunotherapy and chemotherapy to support better outcomes.”
The rapid diagnostic pathway is currently well established for breast cancer while prostate and bowel cancer have just come on stream, and it is planned for the service to be extended in the first quarter of 2023. “We will start covering the lung, the head and the neck over the next three months. But I think that by the middle of next year we should have all of them up and running really well. That’s our aim, to get all those four major cancers, to capture most of the big ones.”
Patel is not just interested in clinical innovations, but also the holistic manner in which the patients are looked after. The clinic offers an impressive array of complementary therapies, including an on-site dietician, physiotherapy, art therapy and reiki. “And when they’re having their chemotherapy and they’re feeling sick, we do reflexology on their feet just prior to their treatment, and for many patients the feeling of sickness almost disappears.

“When they have finished treatment, we have what we call a ‘survivorship programme’,” she continues. “It’s part of the charitable work we do, so we don’t charge. People are never the same after having cancer, and we want them to get back to a normal that they are comfortable with. We want them to feel healthy and have a great quality of life after their cancer.”
Every month the clinic runs a different session on
exercise or nutrition. In the latter, a specialist chef calls the patients into the kitchen to show them how to knock up quick and easy nutritional meals. Another session focuses on sexual and relationship support, overseen by a psychosexual nurse. “For the breast patient, they might have had a mastectomy and they probably don’t know how their partners feel, and they might feel inadequate or unattractive,” explains Patel. “So, it’s about boosting their confidence. For the prostate patients, it’s obviously that they can’t have an erection, certain patients with bowel cancer might have a colostomy bag. How do they manage that with their partners and when they go out socially? Also, how do you go about telling your children that ‘I’ve had cancer’ or ‘I’m afraid of dying’. These are all these very personal matters that can be quite intimidating. So providing help here is crucial.”
Because they can sometimes cover some quite sombre subjects, the psychological session is followed by a course on ‘laughter yoga’ – a combination of breathing exercises from yoga and playful laughing exercises that are based on the principle that your body benefits from laughing even when that laughter is not spontaneous. Laughter is the best medicine, as the old saying goes. “Mainly, though, no one here feels alienated,” says Patel. “And they can share their experiences – almost like a support group.” For someone who is battling cancer, nothing could be more crucial.
Prognosis—59
The London Clinic 20 Devonshire Place London W1G 6BW 020 7935 4444 thelondonclinic.co.uk
When they have finished treatment, we have what we call a ‘survivorship programme. It’s part of the charitable work we do, so we don’t charge. People are never the same after having cancer, and we want them to get back to a normal that they are comfortable with.
MY MARYLEBONE
Eat
Ottolenghi opening up on Marylebone Lane a couple of years ago was one of my best days ever! I love their food and when suddenly there was one so close to work, that was quite wonderful. It was the same with St John, which recently arrived. I think the food there is fantastic. I also like The Italians, up on Blandford Street. It’s a little deli and wine bar, a place to go for light plates.

Work
I am a trained nurse and now ultimately responsible for all the clinical services at Phoenix Hospital Group in London. In Marylebone we have the Weymouth Street Hospital, a short-stay elective care hospital. Then we have 9 Harley Street and 25 Harley Street, which are our outpatient and diagnostic centres. There is not really a typical day for anyone in healthcare, including me. At any moment, I’ve got to be able to jump on issues ranging from a consultant query to a request from the MRI scanning team. My role is to ensure that everything is running smoothly and we are providing the highest level of care safely. That entails looking at everything from a policy perspective and a security perspective. Are we supporting our clinicians in the best way possible? It is also a strategic role and I’m involved in planning what we will be doing in the
longer-term future as well as managing daily operations. As a result of all this, I’m back and forth across all three sites, so I can have a pretty high step count on a good day!
Shop
What’s quite dangerous about working in Marylebone is the fact that there are just so many enticing shops in the area. ME + EM on New Cavendish Street is one of my favourites. There’s also a really beautiful new childrenswear shop called Strawberries & Cream on Wigmore Street. I have a fiveyear-old and there’s always something in there that you can either look at and dream about or buy for an occasion. It’s great for gifts for other people’s children too. Dinny Hall on Marylebone Lane is really lovely, and I really like Paul Smith. But one of the shops that I particularly like, which might sound a little bit odd, is Penton’s,
the hardware store at the bottom of Marylebone Lane. It’s such a wonderful place when you step inside. It’s like its own little world.
Culture
There are some really great galleries in the area. You’re always just a short walk from some wonderful art. There is Clarendon Fine Art on the high street, and I love seeing what new pieces they’ve got in the window. Then there’s Railings Gallery, which again always has some beautiful things hanging up. Wigmore Hall is fabulous, but you have to make a bit more effort to get in there by buying tickets, whereas you can see some really beautiful things just by walking the streets. I love Gallery Eclectic, a really beautiful pottery gallery and shop. I often look in the window. It feels slightly tucked away, you almost don’t realise it’s there, but it’s really lovely.
I recently took my daughter to Cocoro on Marylebone Lane, the Japanese place, and it was just so good. Again, it is one of those under-the-radar places that’s been there forever selling really excellent food. I really love Orrery because of their wonderful rooftop terrace, which is wonderful in both summer and winter. It’s a really nice place to go at night. Then there’s Bonne Bouche, a fantastic patisserie. The quality and variety of food available here is wonderful, if slightly dangerous.
Community
I think Marylebone is probably one of the few parts in London that you really do get that sense of community, because this is otherwise such a big, transient city. Marylebone has got that village feel. It’s nice walking up the street and running into someone that you’ve not seen for a while. You have everything here that you could possibly want, and it’s all very much within walking distance, so you do bump into friends and colleagues. Healthcare is a very small community, so everybody does get to know each other. Even if you don’t live in Marylebone, there is certainly a sense of belonging.
60—Prognosis
PHOENIX HOSPITAL GROUP 020 7079 2100 phoenixhospitalgroup.com
Aleksandra McNee, director of operations at Phoenix Hospital Group

Prognosis—61
WHAT’S ON
MUSIC
SIR MARK ELDER CONDUCTS THE ACADEMY SYMPHONY ORCHESTRA
24th February, 1pm
Royal Academy of Music
Marylebone Road
London NW1 5HT ram.ac.uk
The Academy’s Barbirolli chair of conducting Sir Mark Elder conducts orchestral music from two great 19th-century operas: Verdi’s Aida, set in ancient Egypt, and Wagner’s Tristan und Isolde, based on Gottfried von Strassburg’s early 13thcentury romance and inspired by the philosophy of Arthur Schopenhauer. Strauss’s mighty tone poem, Death and Transfiguration, which depicts an artist’s refections on his life as he dies, completes the programme.

THEATRE
MACBETH: A GOLDEN COUPLE, DESTINED FOR GLORY

15th – 25th February
The Cockpit Gateforth Street London NW8 8EH thecockpit.org.uk
The Macbeths are a golden couple, destined for glory. Admired and feted by all, including the King of Scotland, Macbeth leads Duncan’s forces to a huge military success and crushes rebels and foreign armies alike. The witches, however, can smell his ambition and mendacity. In this provocative treatment of Shakespeare’s masterpiece, they intervene to test Macbeth’s character and loyalty. A disturbing portrait of a man, a woman and a nation in crisis.
EXHIBITION
MHAIRI MCGREGOR: ACROSS THE POND
2nd – 18th March
Thompsons Gallery
3 Seymour Place London W1H 5AZ thompsonsgallery.co.uk
Mhairi McGregor has gained acclaim for her highly abstracted, contemporary colourist landscape paintings. The artist travels the world capturing breathtaking views with her paintbrush. As a young artist, McGregor’s inspiration originated from textiles, practiced and taught by her mother at Glasgow University, and the work of French-Russian painter Nicolas de Stael. Bright and vibrant, her landscapes are layered with complexity and depth. Every patch of oil is deliberately placed and deeply considered; the resulting product is effervescent, accomplished and outright beautiful.
MUSIC
SHEKU KANNEH-MASON
15th March
Wigmore Hall
36 Wigmore Street
London W1U 2BP wigmore-hall.org.uk
Despite his youth, cellist Sheku
Kanneh-Mason has developed into one of UK’s most admired musicians – in 2020, he awarded an MBE for services to music at the age of just 21. In this performance, he plays works by Spanish cellist Gaspar Cassadó (1897-1966), and the Cuban Leo Brouwer (born 1939), plus recent works by Welsh jazz and classical pianist Gwilym Simcock and the English Edward Finnis, whose Preludes were premièred by Kanneh-Mason in 2021.
62—Prognosis
Macbeth
Sir Mark Elder
EXHIBITION
PORTRAITS OF DOGS: FROM GAINSBOROUGH TO HOCKNEY

29th March – 15th October
The Wallace Collection
Manchester Square
London W1U 3BN wallacecollection.org
Through carefully selected paintings, sculptures, drawings, works of art and even taxidermy, this exhibition highlights the unique bond between humans and their canine companions across many centuries. Dog portraiture, which emerged as far back the earliest cave paintings, flourished in Britain from the 17th century onwards. Bringing over 50 works of art to Hertford House, Portraits of Dogs presents a broad range of portraiture showing dogs in all their different shapes and sizes.
BAYLEY & SAGE
33-34 Marylebone High Street
London W1U 4QD bayley-sage.co.uk
Bayley & Sage was founded by Jennie Allen in 1997, who opened her first store in Wimbledon Village. Jennie’s commitment to sourcing high-quality fresh foods from specialist suppliers and selling it with a friendly, welcoming service has proven hugely – and unsurprisingly –successful. The Marylebone High Street store, which opened in 2022, is Bayley & Sage’s largest so far, with stunning displays of food upstairs and the fantastic addition of a B&S Abode homewares store in the basement, great for gifts and homewares.
LA FROMAGERIE
2-4 Moxon Street
London W1U 4EW lafromagerie.co.uk
La Fromagerie, a true Marylebone stalwart, started after its owner Patricia Michelson fell in love with a cheese: a Beaufort in Savoie. She founded a cheeseimporting business from her garden shed and it grew from there. While her business has expanded, the ethos is still the same: it’s still a familyrun affair and it’s still about championing small producers, promoting their expertise and telling their stories. The store’s stunning cheese room, manned by expert afineurs, is now complemented by a grocery and deli selling a wide range of high-quality produce.
DAYLESFORD
6-8 Blandford Street
London W1U 4AU daylesford.com
A beautifully designed emporium of fresh, tasty food, all of it produced on Daylesford’s organic farm in Gloucestershire without cost

to the welfare of animals or the detriment of the environment. It’s a sustainable business model in which energy is recycled, production is economical and every thing from packaging to trade comes under one brand. Bread, cheese, vegetables, fruit and meat are delivered daily from the farm.
THE GINGER PIG
8-10 Moxon Street
London W1U 4EW thegingerpig.co.uk
The Ginger Pig is a proper butcher’s shop. At its heart is respect for the animals that provide the meat and for the skills of the butchers who prepare it. The meat is sourced from a network of like-minded farmers, who between them raise a wonderful array of native British rare breed livestock, with an emphasis on good animal husbandry and welfare. The exceptional meat is skilfully butchered and properly hung on site when appropriate, leaving nothing to waste – the offal, sausages, pies and legendary sausage rolls are as prized as the prime cuts.
PAUL ROTHE & SON
35 Marylebone Lane
London W1U 2NN
Paul Rothe and Son was born on Marylebone Lane on 2nd August 1900 as a German deli. Now, having passed down through three generations of Rothes, it is the quintessential English cafe and pantry. The wursts and sauerkrauts made way for English preserves and condiments. A deli counter sells soups and sandwiches, while the shelves are packed with jars of jams, honeys and pickles sourced, most of them sourced from small producers. Despite the change in products, the store still projects an old-world aesthetic and an undimmed commitment to personal service.
Prognosis—63
Village food shops
David Hockney
Bayley & Sage
THE GUIDE
Places to have a spa day in Marylebone
CHUAN SPA
As part of The Langham, London, the world’s first ‘Grand Hotel’, Chuan Spa aims to maintain a long tradition of luxury and customer service. The treatments offered are centred on the Chinese idea of the five natural elements: wood, fire, earth, metal and water. With exotic names such as Chuan ritual, lavender dream, Chuan harmony massage and Chinese cupping therapy, the idea of the wide range of treatments is to nurture, balance and restore. The spa’s experienced therapists are there to help you embark on a journey

of self-discovery, as well as leaving you feeling refreshed and energised.
CHI YU WELLNESS CENTRE
Chi Yu is a Japaneseinspired wellness centre that provides a variety of complementary therapies and treatments. These include massage therapies, reflexology, acupuncture, aromatherapy, facials and craniosacral therapy. Tailor your treatment according to your needs, combining different therapies to promote and support your wellbeing. Chi Yu offers some less well-known
The treatments offered at Chuan Spa are centred on the Chinese idea of the five natural elements: wood, fire, earth, metal and water.
treatments such as jadebamboo massage, yin yang stone therapy and oriental aromatherapy. The aim is to provide you with somewhere to relax after a hard day’s shopping or de-stress after a busy day at work.
BAKER STREET BEAUTY
Friendly, efficient staff trained in the latest techniques and products will strive to make you feel comfortable all through your visit to Baker Street Beauty. The salon offers luxury facial therapies and different styles of massage such as deep tissue massage, Indian head massage and Swedish massage. You can also treat yourself to a manicurepedicure, or even sharpen up your eyebrows with some threading to ensure you leave looking and feeling your best.
THE LANDMARK LONDON
The beautiful Landmark London hotel on Marylebone Road refers to its sensual spa and health club as places to “nourish the body and mind”. The facilities include four treatment rooms, a state-ofthe-art gym, one of London’s few chlorine-free 15-metre indoor swimming pools, a jacuzzi and a sanarium. Swim, steam and exercise away the stress, or indulge in exclusive body treatments. The spa and wellness centre feature an array of facilities and treatments for relaxation, exercise and enjoyment.
MARYLEBONE THAI SPA
This Thai massage spa on Paddington Street brings the relaxing techniques of ancient Thailand to Marylebone. This tranquil spa, which feels completely at home among the area’s fashion boutiques, quirky bookshops and fine eateries, offers customers a few moments of relaxation using several different Thai massage techniques, designed to refresh and reinvigorate.
64 – Prognosis

The centre of medical excellence in the heart of London harleystreetmedicalarea.com
Answers. Sooner.
Mayo Clinic Healthcare turns scientific discoveries into promising treatments faster, so patients get to the care they need sooner. By combining our expertise in London with the expertise in the United States, we can partner with you to deliver the best care to patients and deliver answers needed.

To learn more visit mayoclinichealthcare.co.uk










































































