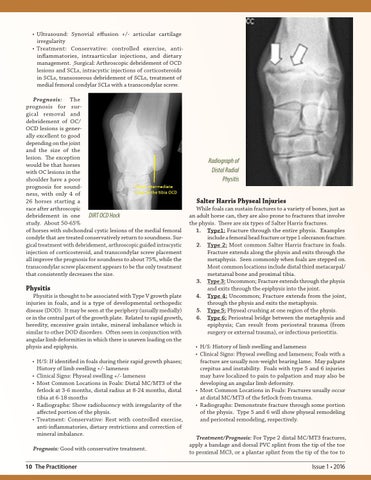
• Ultrasound: Synovial effusion +/- articular cartilage irregularity • Treatment: Conservative: controlled exercise, antiinflammatories, intraarticular injections, and dietary management. Surgical: Arthroscopic debridement of OCD lesions and SCLs, intracystic injections of corticosteroids in SCLs, transosseous debridement of SCLs, treatment of medial femoral condylar SCLs with a transcondylar screw. Prognosis: The prognosis for surgical removal and debridement of OC/ OCD lesions is generally excellent to good depending on the joint and the size of the lesion. The exception Radiograph of would be that horses Distal Radial with OC lesions in the shoulder have a poor Physitis prognosis for soundness, with only 4 of 26 horses starting a Salter Harris Physeal Injuries race after arthroscopic While foals can sustain fractures to a variety of bones, just as debridement in one DIRT OCD Hock an adult horse can, they are also prone to fractures that involve study. About 50-65% the physis. There are six types of Salter Harris fractures. of horses with subchondral cystic lesions of the medial femoral 1. Type1: Fracture through the entire physis. Examples condyle that are treated conservatively return to soundness. Surinclude a femoral head fracture or type 1 olecranon fracture. gical treatment with debridement, arthroscopic guided intracystic 2. Type 2: Most common Salter Harris fracture in foals. injection of corticosteroid, and transcondylar screw placement Fracture extends along the physis and exits through the all improve the prognosis for soundness to about 75%, while the metaphysis. Seen commonly when foals are stepped on. transcondylar screw placement appears to be the only treatment Most common locations include distal third metacarpal/ that consistently decreases the size. metatarsal bone and proximal tibia. 3. Type 3: Uncommon; Fracture extends through the physis Physitis and exits through the epiphysis into the joint. Physitis is thought to be associated with Type V growth plate 4. Type 4: Uncommon; Fracture extends from the joint, injuries in foals, and is a type of developmental orthopedic through the physis and exits the metaphysis. disease (DOD). It may be seen at the periphery (usually medially) 5. Type 5: Physeal crushing at one region of the physis. or in the central part of the growth plate. Related to rapid growth, 6. Type 6: Periosteal bridge between the metaphysis and heredity, excessive grain intake, mineral imbalance which is epiphysis; Can result from periosteal trauma (from similar to other DOD disorders. Often seen in conjunction with surgery or external trauma), or infectious periostitis. angular limb deformities in which there is uneven loading on the physis and epiphysis. • H/S: History of limb swelling and lameness • Clinical Signs: Physeal swelling and lameness; Foals with a • H/S: If identified in foals during their rapid growth phases; fracture are usually non-weight bearing lame. May palpate History of limb swelling +/- lameness crepitus and instability. Foals with type 5 and 6 injuries • Clinical Signs: Physeal swelling +/- lameness may have localized to pain to palpation and may also be • Most Common Locations in Foals: Distal MC/MT3 of the developing an angular limb deformity. fetlock at 3-6 months, distal radius at 8-24 months, distal • Most Common Locations in Foals: Fractures usually occur tibia at 6-18 months at distal MC/MT3 of the fetlock from trauma. • Radiographs: Show radiolucency with irregularity of the • Radiographs: Demonstrate fracture through some portion affected portion of the physis. of the physis. Type 5 and 6 will show physeal remodeling • Treatment: Conservative: Rest with controlled exercise, and periosteal remodeling, respectively. anti-inflammatories, dietary restrictions and correction of mineral imbalance. Treatment/Prognosis: For Type 2 distal MC/MT3 fractures, apply a bandage and dorsal PVC splint from the tip of the toe Prognosis: Good with conservative treatment. to proximal MC3, or a plantar splint from the tip of the toe to 10 The Practitioner
Issue 1 • 2016