in the foot being vulnerable to infection. The early detec tion of the clinical signs of infection in the diabetic foot includes the evaluation of the foot for bone infection. The possibility of bone infection is significantly greater if there is a several weeks’ presence of soft tissue infection or fistula. Plain film radiography of the foot can usually show the bone exposure and signs of osteomyelitis. Primary phase or acute state can show bone demineralisation, diffuse lytic changes on the bone, localised circular changes or confluent changes, with or without sclerotic parts of the bone. Chronic osteomyelitis form comes with sequestra and with more expressive sclerotic and osteolitic parts of the bone. There are several clinical signs of osteomyelitis: swelling and the ’sausage’ look of the finger; probe-to-bone test; deep ulcer. Laboratory indicators of infection are higher sedimen tation of erythrocytes (SE), higher number of leukocytes, C-reactive protein (CRP), procalcitonin, bacteriologi cal smear examination, bone biopsy for bacteriological and histological examination, repeated radiographic ex amination, bone scintigraphy (99mTc diphosphonate), labelled autologous leucocyte scanning (111In oxine or 99mTc-HMPAO), antigranulocyte scintigraphy (AGS), computed tomographic (CT), and magnetic resonance imaging (MRI)3,7,8.
Therapeutic strategies: Literature describes various approaches to osteomyelitis healing in diabetic foot. Surgical exploration of infected part of the bone and bone resection until reaching the healthy part are marked as the traditional surgical ap proach. The advantages of this surgical approach are radi cally removing the bone changed by infection and faster healing. The disadvantages are more bone removed than necessary, possible disturbance of the foot biomechanics, and greater surgical procedure. Conservative surgery in osteomyelitis healing in dia betic foot is an approach in which only the sequestra are removed with very limited bone removal. The advantage of this kind of healing is greater savings but the risk is longer healing times. Healing supported by the use of dressings and followed by systemic antibiotic therapy, can achieve the wanted result of healing even in 85% of osteomyelitis. Healing by antibiotics alone prolongs healing time to/by 12-24 weeks3.
AIM: The aim of this study is to evaluate the surgical proto col applied in treatment of bone infection and chronic wounds, which are related to bone infection in the treat ment of diabetic foot ulcers.
8
a
b
c
d
e
f
g
h
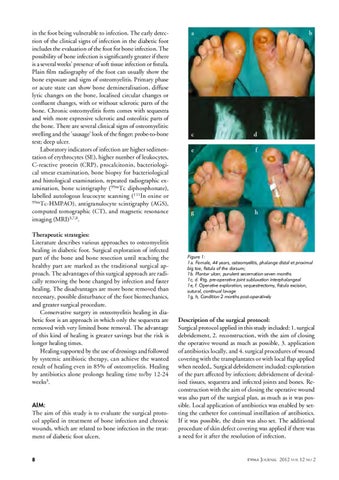
Figure 1: 1a. Female, 44 years, osteomyelitis, phalange distal et proximal big toe, fistula of the dorsum; 1b. Plantar ulcer, purulent secernation seven months 1c, d. Rtg. pre-operative joint subluxation interphalangeal 1e, f. Operative exploration, sequestrectomy, fistula excision, sutural, continual lavage 1g, h, Condition 2 months post-operatively
Description of the surgical protocol: Surgical protocol applied in this study included: 1. surgical debridement, 2. reconstruction, with the aim of closing the operative wound as much as possible, 3. application of antibiotics locally, and 4. surgical procedures of wound covering with the transplantates or with local flap applied when needed,. Surgical debridement included: exploration of the part affected by infection; debridement of devital ised tissues, sequestra and infected joints and bones. Re construction with the aim of closing the operative wound was also part of the surgical plan, as much as it was pos sible. Local application of antibiotics was enabled by set ting the catheter for continual instillation of antibiotics. If it was possible, the drain was also set. The additional procedure of skin defect covering was applied if there was a need for it after the resolution of infection.
EWMA Journal
2012 vol 12 no 2