Suzanne

Greetings Reader!
Welcome to the newest issue of Living with Lupus, published by the Lupus Foundation of America, Greater Ohio Chapter. I’m Suzanne Tierney, President & CEO, and it is both an honor and a privilege to connect with you in these pages once again.
Each time we gather to publish this magazine, I am reminded of the strength, courage, and resilience of our community: those living with lupus, the caregivers, families, friends, medical professionals, advocates - every one of you who makes this journey together. I know that lupus is never a “one-size-fitsall” story. It’s complex, sometimes frustratingly mysterious, sometimes painful, yet always filled with moments of perseverance and hope.
In this issue, we explore the unpredictable journey of lupus. We dive into how to find moments of peace amidst chaos by offering insights into coping with mental health, what happens when life doesn’t go as planned, and updates on research. We also share inspiring stories from people like you - individuals who are living fully despite their challenges, finding support, and holding on to hope for better treatment(s) and, ultimately, a cure.
My hope is that when you turn each page, you feel less alone. I hope you find insights you can use, inspiration to keep going, reminders of how far we’ve come - and why your voice, your experience, and your hope are so essential in this fight.

Please remember: the Chapter is here for you. Whether you need information, advocacy, or simply someone to listen to, our team is ready. Reach out, share your story, ask the questions. Your involvement powers awareness, fuels discoveries, and helps solve what we call “the cruel mystery” of lupus.
Thank you for being part of our community, for your courage, your questions, your stories - and your commitment to living with lupus on your terms. Together, we are moving forward and are dedicated to living our best lives in the midst of the storm.


Suzanne Tierney President & CEO
Lupus Foundation of America, Greater Ohio Chapter
Pg. 1-2 Letter from Suzanne
Pg. 4-5 Patient Navigator Corner: September 2025
Pg. 6-8 Patient Story: Latasha Adams
Pg. 9-11 Patient Story: Lillian Newbern
Pg. 12-15 Research & News
Pg. 16-18 Walk to End Lupus Now® Recap
Pg. 19-21 Coping with the Mental Health Impacts of Lupus, By Heather Rose Artushin, LISW-CP
Pg. 22-24 What Happens When Life Doesn’t Go As Planned? By Chris Milazzo
Pg. 25 Blog & Podcast
Pg. 26-27 Get Involved & Ways to Give
Pg. 28-29 Could You Have Lupus?
Pg. 30 Staff Page


6-8
Patient Story: Latasha Adams 911
Patient Story: Lillian Newbern

2224 1921 Coping with the Mental Health Impacts of Lupus By Heather Rose Artushin, LISW-CP
What Happens When Life Doesn’t Go As Planned? By Chris
Milazzo

PATIENT NAVIGATOR CORNER
SEPT 2025 | BY RITA PICCIN

Political, social, and economic developments are impacting all of us, and the Lupus Foundation of America, Greater Ohio Chapter is no exception. We are experiencing a storm of change. Pharmaceutical and government grant funding has not been renewed, and this reduction in funding has severely impacted our programs and services. This includes the Patient Navigator (PN) and Patient Assistance Programs.
Patient Navigator (PN) Program
As lupians know all too well, lupus can create a chaotic and overwhelming environment for both patients and their caregivers. PNs play a role in helping individuals manage the complexities of living with lupus, providing essential support that fosters a sense of peace and stability. Most unfortunately, the Greater Ohio Chapter’s statewide PN program has been temporarily suspended, and regional PN contracts have not been renewed due to the elimination of state funding. In order to understand how the loss of funding has affected this program, it is important to show the work the PNs have done, and the impact we have had.
During the past 2 years:
• PNs have contacted 2,011 lupus warriors, 43 caregivers and 37
professionals through wellness calls and by responding to inquiries that the chapter receives.
• Contact methods consisted of phone calls, emails, voicemails, texts, mailings and in-person communication for a total of 12,400 touchpoints (an average of 6 per constituent).
• Over 17,100 information/resources were given or requested, including:
• Patient Assistance Programs
• Patient Education Given by Mail
• Patient Education Given by Phone
• Emotional Support
• Patient Updates
• Physician Directory
• LFA, GOC Website Link
• Support Groups
• New Patient Education Class
• Events Calendar
• Educational Programs
• Medication Information
• Financial Resources
• Inquiry Packets
• Patient Toolkit
• Living With Lupus Magazine
• Chapter Newsletter Sign-Up
• Other - resources provided by other agencies, such as housing, rent, utilities, disability, health insurance, Medicare/ Medicaid, etc.
Assistance Programs
The Patient Assistance Programs have also been suspended due to loss of continued funding. The programs aimed to remove barriers to lupus care by providing assistance with food, medical expenses, transportation, and mental health counseling. We were able to provide assistance to 148 Ohio lupians:
• 62% received food assistance in the form of grocery store gift cards.
• 20% received reimbursements for out-of-pocket healthcare expenses.
• 10% received referrals to Signature Health for mental health counseling.
• 8% received ride assistance through Uber Health to and from healthcare appointments.
Thank You to Our Wonderful Patient Navigators!!!
We could not have reached so many lupus warriors throughout the state without the dedicated efforts of the regional PNs. As Suzanne Tierney writes, the PNs “. . . should all be proud of the work you have done. We collaborated during the pandemic to ensure that our Ohio lupus patient population received the care and resources they needed. You identified patients who needed additional help and referred them to our Lead PN for support services.
You worked in your communities to garner city and county proclamations for Lupus Awareness Month. You appeared on radio and TV programs to educate the public about lupus. You attended many health fairs and community events to create awareness and identify patients who may not be aware they have lupus. You have all done an incredible job working towards a better future for people with lupus.”
Brenda Angle
Lisa Breiding
Allison Fedon
Renee Lyons
Halli Martin
Aaron Meller
Justina Patterson
Nikki Roberts
Samantha Sebestinas
Mike Vollmar
We Are Committed to Supporting Lupus Warriors
As the lead patient navigator, I am still committed to providing education and support to patients, caregivers, and professionals. Without the wonderful regional PNs, I will not be able to reach as many people as we did in the past. However, I am still available to help Ohio lupians understand lupus and manage living with the disease. If there are needs or resources a lupus patient may have which we cannot provide, I can research other agencies and organizations that may be able to
help. The Greater Ohio Chapter is dedicated to finding other sources of funding to bring back the Patient Navigator and Assistance Programs, in addition to potentially creating new programs to help lupus warriors and caregivers.
Although the future is uncertain, please know that we are doing our best to continue providing education and support. But, we can’t do this alone. There is no “I” in lupus, only “us.” Please help us, help you. Consider donating, volunteering, and advocating for the chapter. If you have questions or would like information, please contact the Greater Ohio Chapter office at 1 (888) NO-LUPUS, 440-717-0183, or info@lupusgreaterohio.org.


PATIENT STORY
Living with Lupus: A Journey of Resilience, Faith, and Finding Purpose in Pain
November 1, 2000. That date is etched in my memory as the day my life changed forever. It was the day I received my lupus diagnosis, and with it, a sentence that would test every fiber of my being: “You may not live to see 30.” I was young, vibrant, and full of life. I had been extremely active, flexible, and energetic – the kind of person who embraced each day with enthusiasm. In an instant, that all changed as fatigue and relentless pain became my new reality.
The transformation was swift and devastating. Within two months of starting treatment, which included nearly 30 medications – steroids and chemotherapy among them –my body became unrecognizable to me. The steroids caused me to balloon from a size 3-4 to a size 16-17. I was so embarrassed that I avoided going outside. When people would ask if I was Latasha Adams, I would lie and say no, unable to face the shock in their eyes. The vibrant, confident woman I had been seemed to disappear beneath layers of medicationinduced weight gain and the invisible burden of chronic pain.
The Chaos of Chronic Illness
Living with lupus means living

with uncertainty. Each day brings the possibility of a flare-up that can derail even the best-laid plans. On my most difficult days, I come home from work and go straight to bed. The pain radiating through my body is so severe that my blood pressure skyrockets to stroke-level numbers. People can see it in my face when I’m suffering – there’s no hiding the toll this
disease takes. But lupus didn’t come alone. Over the years, I’ve been diagnosed with fibromyalgia, sciatica, rheumatoid arthritis, degenerative disc disease, and acute myofascial chronic pain syndrome. It’s as if my body became a battlefield where multiple conditions wage war against my peace and comfort. The pain became so unbearable that
it affected every aspect of my life, including my relationships. Where I had once been sexually active and enjoyed physical intimacy, I couldn’t bear to be touched. The pain made me withdraw from the world and from the people I loved.
In 2012, when pain medications were taken away from patients like me, I found myself suffering in ways I never imagined possible. I was bedridden, unable to walk, watching life pass by from my bedroom window. The Cleveland Clinic tried to help with injections through pain management, but when those failed, they told me surgery was my only option— something I rejected. I was at my breaking point, desperate for relief and answers.

“This passion (cooking), inherited from my beloved grandmother, doesn’t take the pain away, but it eases it.”

Finding Light in the Darkness
Sometimes help comes from unexpected places. My rheumatologist, Dr. Van Warren, referred me to a ketamine specialist, but while waiting for that appointment, I took matters into my own hands. Through my own research, I discovered Dr. Leon Margolin, MD, PhD, a medical and interventional pain management doctor based in Columbus, Ohio, who also practices in Warrensville Heights. Dr. Margolin was different – he listened, he cared, and he understood that behind every patient was a human being desperate for relief. The process was lengthy, but it was worth every step.
When the unpredictable symptoms hit, I’ve learned to cope by fo -
cusing on what I love most: cooking. This passion, inherited from my beloved grandmother, doesn’t take the pain away, but it eases it. When I’m in the kitchen, concentrating on perfecting a dish or creating something new, the pain recedes into the background. It’s my form of meditation, my escape, and my way of channeling something positive from the chaos.
As a chef, I work on my feet for long hours – often over 55 hours a week now. I always inform employers about my condition upfront, and thankfully, most have been accommodating. I wear comfortable shoes and compression socks, and I always ask for a mat and chair in case I need to sit. It’s about finding ways to adapt without letting the disease define my limitations.
The
Power of Community and
Support
One of the greatest blessings in my lupus journey has been discovering the Lupus Foundation of America, Greater Ohio Chapter. This organization has been a lifeline in ways I never expected. They’ve
recognized my contributions to the lupus community, introduced me to support groups, and regularly check on my family’s well-being. When I’ve needed resources— whether for food, transportation, medications, or referrals—they’ve been there. Their recognition dinners and grants have reminded me that I’m not alone in this fight.
But I’ve also been blessed with a circle of people who see beyond my strength to the vulnerable person underneath. My fiancé, Seymour Sweeney, my favorite cousin Teresa Lynn Colberts, and my best friends who I consider family – Melissa Bentley, Katrina Richardson, Irisa McCray, and Darion Smedley – these are the people I can call when the pain becomes overwhelming. They’ll sit there while I vent and cry, knowing how rare it is to see me break down because they know how strong I usually am.
At work, I’ve been blessed with two ladies who I welcome as sisters – Ebony Bell and Tran Bui. Not a day goes by without them checking on me each morning. I hold them dear to my heart because they help my days go by smoothly, and I so appreciate their consistent care and concern. Additionally, I found a naturalist at my job named Niri, who has been truly an inspiration. She is always helpful with natural products and natural healing, offering an alternative perspective on wellness that complements my traditional medical treatment.
Having people who will simply witness your pain without trying to fix it or judge it, others who make your daily struggles more manageable, and those who introduce you to new ways of healing is invaluable. The Lupus Foundation, Greater Ohio Chapter taught me that having a support system isn’t a luxury—it’s essential for survival. If you don’t have family or friends who understand, organizations like the Greater Ohio Chapter become

your chosen family, connecting you with people who truly get what you’re going through because they’re living it too.
Strategies for Survival and Growth
Through years of trial and error, I’ve developed strategies that help me not just survive, but thrive. Remaining calm under pressure is crucial because stress triggers flare-ups. I’ve learned to be kind and patient with myself, understanding that some days will be harder than others. Helping others when I’m able gives my pain purpose—it transforms my suffering into something meaningful.
I stay away from negativity like it’s poison because it is, especially for someone with an autoimmune condition. I educate others about lupus whenever possible, breaking down misconceptions and sharing real experiences. Most importantly, I’ve learned to live my life despite the disease, not because of it. I’ve also become more open to exploring both traditional medicine and natural healing approaches, understanding that wellness can come from many different sources.
A Message of Hope
To anyone newly diagnosed or struggling with lupus, I want you to know that the doctors’ predictions don’t have the final word – God does. When they told me I might not live to see 30, I got
depressed, but I also got determined. I have three children who need me, and I knew no one would love them the way I do. Now I also have three beautiful grandbabies – RyLee Colbert, Tru Colbert, and Amia Adams – who give me even more reasons to keep fighting and thriving.
There were years when I couldn’t work, couldn’t hold a job due to pain, was out of shape, and endured people making fun of me. But I kept my faith and put God first. Today, I’m not just working –I’m thriving, putting in those 55+ hour weeks that seemed impossible just a few years ago.
Never give up. Keep the faith. If God did it for me, He will do it for you. And remember, if you can’t find the strength to keep going, I’ll keep fighting for all of us. We are not victims of lupus – we are trophies, proof that the human spirit can overcome even the greatest challenges.
God gives His greatest battles to His toughest soldiers, and we are winning this war, one day at a time. I love you all, and I’m praying every day that researchers find a cure. Until then, we stand together, supporting each other through the chaos and pain, finding beauty and purpose in our shared journey of resilience.

PATIENT STORY
Lillian Newbern’s Lupus Story
Hi, my name is Lillian Newbern. Everyone calls me by my middle name, Jamaica. I am a single mother. Also, I have lupus. In 1997, my world changed because I was diagnosed with SLE. This was the start of a new journey for me. I quickly learned that one does not have to look a certain way to be sick. And, I was the perfect example.
So, one day I went from being a single working mom to being sick in a blink of an eye. It started at work. I had spilled something that was not closed tightly inside a tote at work. My hand had started to itch real badly. I was having an allergic reaction.
So, I left work and went straight to the ER to get it looked at. My hands were red and burning so bad. Grant Hospital here in Columbus, Ohio, told me that I was probably having an allergic reaction. I gave the ER a short version of what all happened while I was at work. They started running a lot of tests. I also had a fever, and they needed to get that down.
My fever went down some. They came back and told me that the tests didn’t show anything bad. So, they gave me some prescriptions for some creams to help with the itch. I went home, but my fever went back up. I was drained and in some pain. Then my grandma told me to go back to the ER. But, this time to go to The Ohio State University. And, that is what I did. I always listened to my grandma. She knew best.
When I got to OSU, they checked me in and took me back quickly because they said my fever was too high. And, all of the tests began. I told them the story that I told Grant hours before. It was a waiting game to see the results of the tests. When the test results all came back, I was told I have an autoimmune illness. And, it was probably lupus. So, a plan was set.
I was put on a lot of meds. My state of mind was all over the place. Talk about all the crying I did, knowing I was really sick, and I still had a child to raise who needed her mom. All I could do now in my life
was have faith in God. And to try to stay strong for myself and my daughter.
I looked in the mirror and said, “Jamaica, you got this. You got this child who needs you.”
I started to read up all about lupus. Because I knew this would be hard to deal with. But giving up was never an option for me at all. Just a redo in my life was making me believe that I just needed to change some things around.
Thinking back to while I was growing up, I was always a sick child. I would stay home, getting colds a lot. My immune system was always weak. At the age of 12, my appendix ruptured, and I had to go to the hospital to get it removed.
The medications I was put on made me upset to my stomach. I started to lose weight. I was getting weak. But, I just prayed to get better. My grandma would pray for me to heal. And, I knew I would be good for sure as long as I had her praying for me.
I started to get more joint pain, and red patches on my face and arms, that would be red or bleed some days. It was hard to deal with all the trips to different doctor appointments. It was starting to take a toll on me for sure. The tests - all the blood draws, EKG’s, breathing tests, eye appointments, and MRI’s would take over my life now more than ever. But I kept showing up and fighting to stay alive.
When medicines would no longer work, my doctors would try something new. Some meds worked and some didn’t at all. I had started to see my hair thin out. And, I loved my long hair for sure. But I was not really upset about my hair. Because I was still alive. Years have passed, and I am still here to tell my story. I had even started dating for a while. But, my illness had stopped me from doing this in the past.
I decided to focus more on my illness again. But to my surprise, the relationship had not fully ended. And, I found out that I was pregnant with my second child. I was happy and scared at the same time, because I had read that lupus could really harm me or my child during pregnancy.

So, I had to be careful. I just prayed and asked God to let me get through this all. I had to stop some of my meds. My team of doctors helped me get through it all. And, I had a beautiful baby girl. My lupus never even messed with me the whole time I was pregnant. My lupus was so calm. I was enjoying life again after years of back and forth to the ER, hospital stays, and

all the pain and rash flare-ups. I was feeling so great.
I did have some ups and downs over the years. I finally knew what to do when my lupus would flare up. I was teaching myself how to deal with my lupus more. I read up on lupus more and more. Dealing with lupus was just a test for me, against all odds, that I could live with it and be normal.
I set a new plan for my life, and it was working. My fear was finally over. I started to go outside more. I took control of my life again. Now, in the past, I would be so stressed and depressed and would keep only to myself and my kids. I would not hang out with friends or family at all because they just didn’t understand what my lupus was doing to my body or frame-of-mind either. And, the more I was asking them to educate themselves on lupus, they just would not, so that was no support to me at all.
I worked hard with my doctors to get me the best help there was. I started on Benlysta treatment. It

has been a few years now. I love it, and it works for me. My skin has cleared up a lot.
Now, I am having a slight nerve problem. But, I am dealing with it. My lupus is stable for the most part. I have walked three lupus walks in Columbus. I plan to walk as many as I can. I met some new lupus patients, and we are friends now. I try to join as many virtual lupus webinars as I can. I have a lupus group on facebook now, where I share my days, appointments, or anything I find out about lupus.
The Lupus Foundation of America, Greater Ohio Chapter has helped me so much over the years, since I have been linked with them. I am blessed to be able to benefit from the services they have offered lupus patients here in Ohio. I appreciate it all, I really do.
Also, I have been doing a lot for the lupus community. I did a poster for the lupus clinical trials with
in pain, and all. I just walked with the Lord, and He held my hand the whole way through it all.
I can say I have grown to be a better person. I put my mind to something and I get the job done. Not only am I fighting to stay alive and deal with lupus, I have children and a granddaughter to live for now.
I adore my kids and family so much. And, this is why I shall continue to take care of my health first so that I can live to overcome lupus.
“I put my mind to something and I get the job done. Not only am I fighting to stay alive and deal with lupus, I have children and a granddaughter to live for now. “
my dermatology doctor. When I meet new people, I tell them about lupus also. I am just spreading the word.
Right now, I am writing my own books about me and my lupus. I’ve also been giving blood samples to the hospital for more research. I am so proud to help advocate and do what I can for lupus. I feel famous nowadays, when people and nurses say they’ve seen my poster for clinical trials at The Ohio State University location.
I want people to know lupus doesn’t define me at all. Yes, I am sick, but I am also living with a purpose. At the age of 49, I’ve come a long way from 1997. I was blessed to raise my children and other children over the years while dealing with my lupus.
This has been a roller coaster ride for sure with ups and downs along the way. But, I held it all down. This long journey in my life has shown me a lot. I did it sick, tired, drained,


Research, News, & Updates
Study Explores Preload Deficiency in People with Systemic Lupus Erythematosus
Inside Lupus Research (ILR): Disease Management News
A new study suggests preload deficiency could be the underlying cause of fatigue and exercise intolerance in people with systemic lupus erythematosus (SLE). Preload deficiency is a condition where the heart’s capacity to fill with blood before pumping (preload) is reduced, leading to symptoms like fatigue and exercise intolerance. Exercise is particularly helpful for people with lupus, and most people with lupus can take part in some form of activity.
A group of 10 women with SLE with debilitating exercise intolerance was studied. The women did
not have anemia, active SLE, or other conditions that would cause debilitation. Various cardiac and blood tests were conducted on the women. All study participants showed reduced exercise tolerance, and in five participants, right heart catheterisation during exercise confirmed preload deficiency. To address this, participants were advised to increase fluid intake (to 128 oz/day), increase sodium intake (to more than 5 g/day), and use compression stockings. Ivabradine was added to the regimen when fluids and sodium were not sufficient or tolerated.
All participants reported improvement in symptoms. Additionally, the study participants also had
low or undetectable NT-proBNP concentrations (a protein released by the heart under stress) which the researchers believe could be a potential biomarker for preload deficiency.
These findings highlight a potentially treatable cause of fatigue and exercise intolerance in some people with SLE. Future research is needed to determine preload deficiency’s prevalence and understand its role in SLE. Learn more about staying active when you have lupus.
This post was originally published on this site: http://bit.ly/45p4zMm

Systemic Lupus Erythematosus-Specific Risk Factors Linked to Osteoporosis and Bone Fracture Development
Inside Lupus Research (ILR): Disease Management News
In a new study, systemic lupus erythematosus (SLE) disease severity indicated by the presence of lupus nephritis, (LN, lupus-related kidney disease) and other SLE risk factors contributed to reduced bone mineral density (BMD) and an increased risk of osteoporosis.
People with SLE are at higher risk of fractures and osteoporosis, and the impact of disease-related factors on bone health is unclear.
The data of 110 individuals with
SLE who were either currently or previously treated with glucocorticoids were examined. Researchers looked at BMD and osteoporosis-related factors. They found that 41% of participants had osteoporosis, and 29% of the cohort had major osteoporotic fractures, plus 35% of participants had LN. Lower BMD was associated with LN (Class III/IV), higher C-reactive protein (CRP), U1-RNP antibodies, and longer disease duration. Overall, osteoporosis was associated with LN, older age, higher health assessment questionnaire scores, and complement factor 3 levels.
This study highlights the importance of administering 3D bone structure screenings, such as the Dual-energy X-ray Absorptiometry (DXA) screening, in people with SLE, particularly those with higher disease activity, CRP, LN and U1-RNP antibodies. The study also underscores a need for improved and effective screening strategies in lupus. Learn more about how lupus affects the bones.
This post was originally published on this site: http://bit.ly/46WncbD
New Research by Lupus Foundation of America Identifies High-Impact Solutions to Address Health Disparities in Lupus
The Lupus Foundation of America has published a new study in the latest issue of Arthritis Care & Research identifying high-impact solutions that address inequitable health outcomes in lupus due to adverse social determinants of health.
Addressing health and healthcare disparities linked to negative social determinants of health is a key goal in the management of lupus, as disparities in outcomes can be stark. Increasing the visibility of potential solutions and aligning healthcare professionals, policymakers and patient advocates on top priorities can enable more efficient and effective contributions
to healthcare equity and ultimately improve health outcomes for people living with lupus.
Following LFA’s comprehensive review of potential solutions and initiatives currently underway in the field, they convened an advisory panel of lupus experts to evaluate, further define and classify each recommended solution based on feasibility, impact, and costs.
Through a consensus-based approach that included iterative reviews, in-depth discussions and surveying, the panel aligned on 33 high-impact solutions, which were classified into four key categories: Financial Safety Net, Patient Educa-
tion and Shared Decision-Making, Physician Education, and Other Solutions.
The paper, which can be accessed below, provides a framework for focusing efforts on interventions that can make a meaningful difference and have a high impact on improving the quality of life for people living with lupus.
This post was originally published on this site: http://bit.ly/3JBGt8K

Lupus Foundation of America and Lupus Canada Award Research Grant to Study Aiming to Uncover the Causes of Fatigue in People with Lupus

The Lupus Foundation of America (LFA) and Lupus Canada are pleased to announce Mohamed Osman, MD, PhD, Associate Professor of Rheumatology at University of Alberta, as the recipient of the 2025 Lupus Canada Catalyst Award. His study “Defining the molecular drivers of fatigue in lupus: a pilot study,” aims to uncover the reasons behind severe fatigue that people with lupus often experience, which is frequently linked to pain and brain fog.
Causes of extreme fatigue in lupus are still unknown. Dr. Osman will study whether people with lupus who experience extreme fatigue exhibit elevated blood markers of inflammation, and if inflammation in the blood is a contributing factor to this debilitating symptom. The study aims to better understand the cause of fatigue in lupus, which may result in developing new treatment targets and more effective laboratory tests that can better identify lupus patients with these debilitating symptoms.
“Many people with lupus, regardless of how active their disease is, suffer from severe and debilitating fatigue and yet, the cause of fatigue is not well understood.
Our aims are to identify abnormal molecular pathways related to inflammation and oxidative stress that we think might promote fatigue with the long-term goal to design future studies aimed at developing effective therapies for the fatigue experienced by many lupus patients,” shared Dr. Osman. “The Lupus Canada Catalyst Award from the Lupus Foundation of America and Lupus Canada is instrumental in supporting this important research so that we can work to improve the quality of life for everyone impacted by lupus.”
The Lupus Canada Catalyst Award provides funding for one year to Canadian lupus researchers in any phase of their professional careers to champion novel research that can potentially improve the quality of life for people with lupus.
“Our partnership with Lupus Canada enables us to work together across organizations to fund crucial areas of lupus research,” said Joy Buie, PhD, MSCR, RN, Vice President of Research, Lupus Foundation of America. “The research conducted by Dr. Osman is seeking to understand the causes of extreme fatigue often observed
in people living with autoimmune diseases like lupus. This work is important because fatigue drastically decreases the quality of life for people living with lupus and there are currently no effective treatments routinely used to address this issue in the communities we serve. Findings from this study hold promise for life changing solutions that will help better manage or prevent the debilitating impacts of lupus fatigue.”
“Our partnership with the Lupus Foundation of America allows us to collaborate on funding vital lupus research,” said Leanne Mielczarek, CEO, Lupus Canada. “Dr. Osman’s research focuses on uncovering the underlying causes of the debilitating fatigue experienced by so many living with autoimmune diseases like lupus. Fatigue has a significant impact on quality of life, and with no consistently effective treatments currently available, this study offers real hope for meaningful progress. We are proud to support research that could lead to life-changing solutions for individuals affected by lupus.”
This post was originally published on this site: http://bit.ly/3HqaCa2

The Walk to End Lupus Now® Recap
The Walk to End Lupus Now® is a peer-to-peer fundraiser that happens nationwide. The walk is aimed at creating awareness for the disease, all while creating a space for lupus patients to connect with other patients. The Lupus Foundation of America, Greater Ohio Chapter has been working endlessly for decades now to create a fun environment for patients and caregivers which celebrates lupians and all of their accomplishments.
We first gathered in Columbus on July 26th at the Center of Science and Industry (COSI). While the walk in Columbus was a tad different than last year, the lupus warriors of Ohio showed up and turned the city purple! We set a fundraising goal of $25,000 and unfortunately
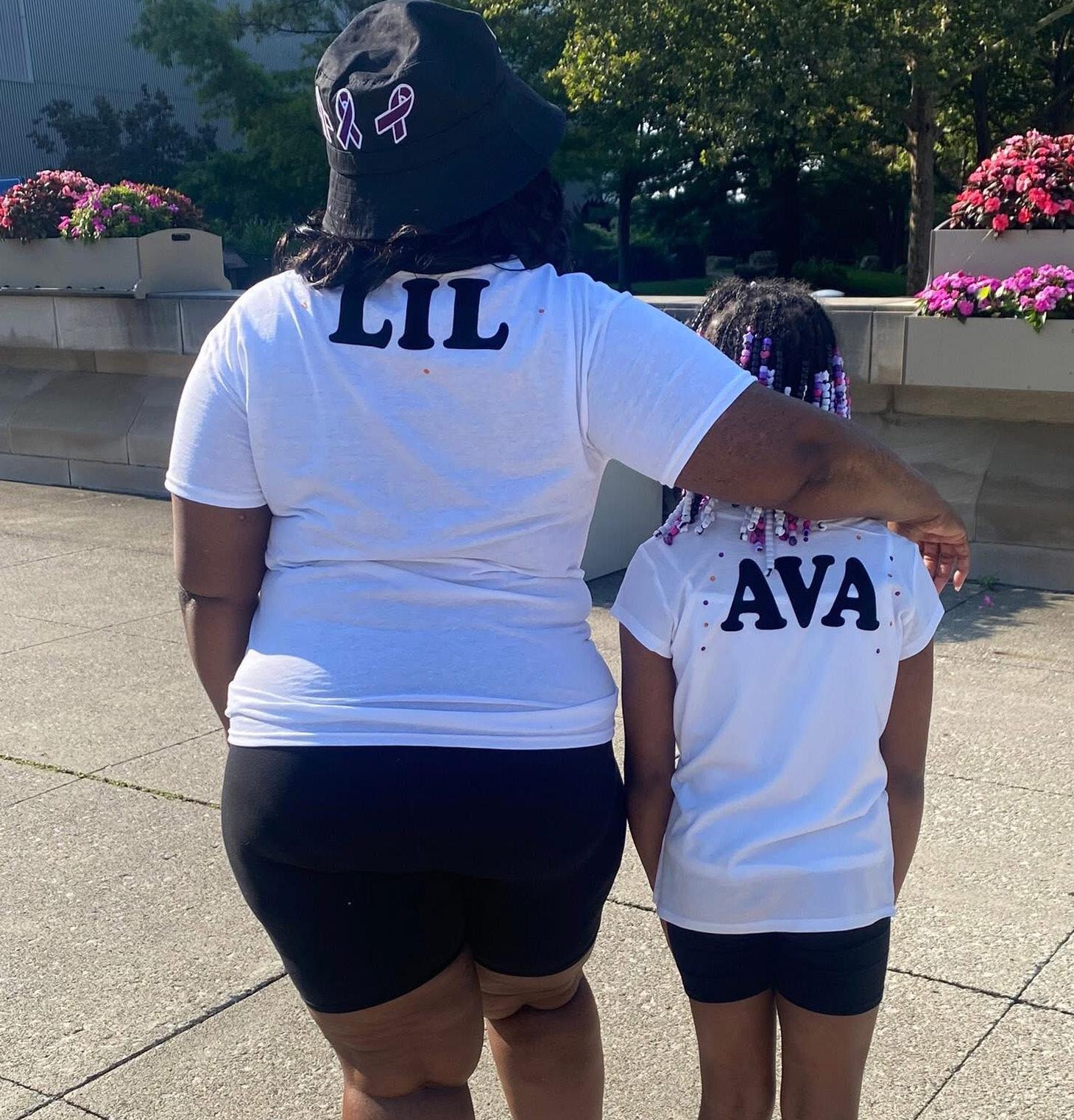
we didn’t make that. WE EXCEEDED IT! We have to give a huge shoutout to our top fundraisers Rosie Chapman and Tiffany Thiede. These two powerhouses brought in nearly $15,000 and we couldn’t be more thankful for their efforts and every single walker’s dedication!
Flash forward to September 6th, where we held the Walk to End Lupus Now® in Cleveland at The Flats East Bank. We met in the beautiful weather to walk towards a lupus-free future! We have to give a big shout out to our top fundraisers, Kelly Perhach, Valerie Tenda, and Terri Patterson Kreider! These three trailblazers brought in a combined $12,000! We couldn’t have done it without them. And, thank you to everyone who registered and walked with us! Whether you walked the butterfly stroll or



the three-mile walk, your support ensures a positive future for lupus patients.
We want to give a big thank you to everyone who participated this year. From the lupus patients, to the caregivers, to the supportive family members and friends, we thank you for taking action in the fight against lupus. While this has


been a year filled with many ups and downs, we all managed to step up and show out! Our walks are not only fundraisers, but a reminder to lupus warriors that you are not in this fight alone. You have a whole army of people behind you fighting the same fight. We thank you for continuing to fight this fight with us.

Coping with the Mental Health Impacts of Lupus
By Heather Rose Artushin, LISW-CP
This post was originally published on the Lupus Foundation of America Website: http://bit.ly/4ns952U
Living with lupus can significantly affect your mental health . . . . More than half of people with lupus experience mental health concerns, from depression to anxiety and beyond, so it’s important to make space for activities that protect your mental health in your day-today life.[1,2]
Here are a few positive coping strategies to help you take care of your mental health while living with lupus.
Stress Management
Research shows that stress contributes to lupus flares and disease activity.[3] Managing stress can be challenging, especially when you’re dealing with debilitating lupus symptoms, work and family changes and other stressful life events. Finding ways to better manage stress can help you to feel better, both physically and emo -
tionally.
Mindfulness has been shown to reduce stress and improve quality of life for people with lupus.[4,5]
Finding a comfortable place to sit, taking a few deep breaths, focusing your attention on the present, and using your five senses to immerse yourself in the sensations of the world around you, can be simple ways to practice mindfulness daily for stress-reduction. A bodyscan meditation, like this one, can also help soothe chronic pain.
Yoga, tai chi and meditation are other approaches to reducing stress supported by research. Regular yoga practice may reduce the intensity of anxiety, and progressive muscle relaxation is a promising intervention for anxiety and depression.[6]
No matter what stress manage -
ment approach works best for you, make it a habit to tune in to your thoughts, feelings and body sensations throughout the day. This can help you to handle emotions, including feelings of stress and anxiety, as they arise. Increasing your awareness can help mitigate stress and let you know when it’s time to reach out for help.
Journaling
Journaling can be a helpful tool when you’re living with lupus. Your journal is a great place to track your thoughts, feelings, symptoms and body sensations when you check-in with yourself throughout the day. The more data you collect in your journal, the better you’ll be able to notice possible triggers that worsen your lupus symptoms so you can avoid them in the future. This information can help you make the most of your medical appointments with your
Using your journal as a safe place to express your emotions can also reduce stress and give you a greater sense of control. In fact, research shows that expressive writing about traumatic, stressful, or emotional events in your life can actually improve both your physical and psychological well-being. [7] Some people living with lupus have also found journaling to bring greater mental clarity and believe it to be a helpful tool in preserving memory in the midst of lupus-related brain fog.
Finding Support
Lupus can be unpredictable at times, so having a clearly-defined support network can give you the practical and emotional support you need on tough days. It can be helpful to map out your support network to remind yourself that you’re not alone on this journey, and to have a plan for when help is needed in the future. Here are a few things to consider when creating your network of support:
1. Consider how you can best support yourself each day. Create a thoughtful self-care plan outlining how you can be your best support person in your daily life. You might commit to a regular bedtime and wake time, create a nutrition plan, schedule a time for journaling and meditation, prayer, or other activities that nurture your mind, body and spirit.
2. Embrace those in your inner circle. The people closest to you – your best friends, family members, partner, etc. – are those that you call upon for emotional support and for practical help when you need it, whether it’s a ride to the doctor’s office, a meal or help with your children when you’re in the midst of a flare. Let the people in your inner circle know how much
you appreciate their love and support and take time to share with them the ways you might call upon them for help in the future as you navigate life with lupus.
3. List your professional support systems. Medical providers and therapists can go on this list, as well as any other support avenues you have available that you can afford to employ when you need it. This might include meal delivery services, house cleaners, babysitters, and other professional helpers you can plan to utilize when needed.
4. Identify those in your outer circle. Friends from church, organizations or sports teams you’re a part of, and people in your neighborhood might fall into this category of support. Consider how they might support you – a neighbor might agree to mow your lawn, or your teammates may take turns checking in with you when a lupus flare keeps you on the sidelines.
5. Get connected to a Lupus Foundation of America support group. The Lupus Foundation of America National Network offers both in-person and virtual support groups across the country. This resource page can help you learn more and get connected.
Energy Conservation
Spoon theory is a metaphor for the energy limitations that people with chronic illnesses, like lupus, face every day. Some days you may have more “spoons” of energy than others, and it can be frustrating and discouraging to find yourself unable to keep up with the things you used to enjoy doing.
One way to plan your energy use is to make a list of all the activities you enjoy. Whether it’s cooking your own meals, playing with your children, volunteering with an organization, or maintaining your garden, what you value most is unique to you. Prioritize your list, putting activities in order of importance. Time and energy management can help you get to the

things that matter most when your spoons of energy are limited.
After taking care of your daily routine – self-care, work commitments, etc. – decide where to spend your remaining energy based on your prioritized list. Living by your values can help you to feel purposeful in where you spend your energy.
Knowing what’s important to you can also give you the strength to say no to commitments that will steal your energy away from what you value most. Setting healthy boundaries around your time and efforts will help you to live a life you love, even within lupus’ unexpected limitations. Saying no to the people we love can be hard – the more you practice respectful boundaries with your health and wellness in mind, the easier those complex conversations will become.
There will be days when you aren’t able to do any of the activities on your list, and that’s okay. We all need to rest and recharge, especially when living with lupus. Listen to your body, and spend your energy with intention, whether it’s a little, or a lot.
Therapy
One of the most important things you can do to protect your mental health when living with lupus is to find a licensed therapist who can support you. Cognitive Behavioral Therapy (CBT) has been shown to be particularly effective in addressing chronic stress in people with lupus.[8]
In therapy, you’ll spend time building trust with your therapist, sharing your story and becoming more aware of your thoughts, feelings and reactions to your lupus symptoms and diagnosis. Your therapist can also support you in navigating the impacts lupus might have on your relationships, your career and other aspects of your life.
Finding the right therapist is important. Start by getting a list from your insurance provider of in-network therapists in your area, and ask your doctor, friends and family for recommendations. Some therapists specialize in working with people facing chronic health issues, while others might be better equipped to meet you where you are in your anxiety or depression. Today, many therapists are available for online therapy sessions, which are especially convenient when you’re not feeling well.
If you meet with a therapist and feel they might not be the right fit for you, don’t give up! There are plenty of therapists out there, each with their own unique background, personality and specialization. Finding a therapist you can confide in and enjoy working with is a gift – keep searching until you find the right therapist for you.
Though lupus can impact your mental health, proactively embracing positive coping strategies can protect your wellbeing and help you feel prepared to manage all the emotions that arise along your journey with lupus. Lean on your support system, find a therapist and tune in to your emotions. You don’t have to navigate your mental health alone!
References
1. Figueiredo-Braga M, Cornaby C, Cortez A, Bernardes M, Terroso G, Figueiredo M, Mesquita CDS, Costa L, Poole BD. Depression and anxiety in systemic lupus erythematosus: The crosstalk between immunological, clinical, and psychosocial factors. Medicine (Baltimore). 2018 Jul;97(28):e11376. doi: 10.1097/ MD.0000000000011376. PMID: 29995777; PMCID: PMC6076116.
2. New Study Found People with Autoimmune Diseases Underreport their Mental Health Status | Lupus Foundation of America. (n.d.). www.lupus.org. https://www.lupus. org/news/new-study-found-people-with-autoimmune-diseases-underreport-their-mental-health-status
3 Jolly M, Katz P. Predictors of stress in patients with Lupus. Front Med (Lausanne). 2022 Sep 29;9:986968. doi: 10.3389/fmed.2022.986968. PMID: 36250087; PMCID: PMC9556948.
4. Molina E, Gould N, Lee K, Krimins R, Hardenbergh D, Timlin H. Stress, mindfulness, and systemic lupus erythematosus: An overview and directions for future research. Lupus. 2022 Nov;31(13):1549-1562. doi: 10.1177/09612033221122980. Epub 2022 Aug 23. PMID: 35998903.
5. Taub R, Horesh D, Rubin N, Glick I, Reem O, Shriqui G, Agmon-Levin N. Mindfulness-Based Stress Reduction for Systemic Lupus Erythematosus: A Mixed-Methods Pilot Randomized Controlled Trial of an Adapted Protocol. J Clin Med. 2021 Sep 28;10(19):4450. doi: 10.3390/ jcm10194450. PMID: 34640468; PMCID: PMC8509215.
6. NIH. (2020, April). Mind and Body Approaches for Stress and Anxiety: What the Science Says. NCCIH. https://www.nccih.nih.gov/health/providers/digest/mind-and-body-approaches-forstress-science
7. Baikie, K. A., & Wilhelm, K. (2005). Emotional and Physical Health Benefits of Expressive Writing. Advances in Psychiatric Treatment, 11(5), 338–346. https://doi.org/10.1192/apt.11.5.338
8. Nuria, Navarrete-Navarrete & Peralta-Ramírez, María & Sabio-Sánchez, J.M. & Coín, M.A. & Ortega, Humbelina & Hidalgo-Tenorio, Carmen & Ortego Centeno, Norberto & Callejas-Rubio, J.L. & Jiménez-Alonso, J. (2010). Efficacy of Cognitive Behavioural Therapy for the Treatment of Chronic Stress in Patients with Lupus Erythematosus: A Randomized Controlled Trial. Psychotherapy and psychosomatics. 79. 107-15. 10.1159/000276370.


What Happens When Life Doesn’t Go As Planned?
By Chris Milazzo, Events Assistant, Lupus Foundation of America, Greater Ohio Chapter
Our family, friends, co-workers, and loved ones can also face burdens and storms. Life impacts all of us. Here is Chris’s story.
I’ve always had a very visual mind. For as long as I can remember, I could picture what I wanted my life to look like. At 5 years old, I imagined myself as a grown-up, falling in love, working my dream job, and starting a family. I liked having a roadmap, a vision to chase after.
But if there’s one thing I’ve learned, it’s that life doesn’t always cooperate with our plans. Nobody grows up thinking, “By the time I’m 30, I’ll have a disease that changes the entire trajectory of my life,” or, “In a few years, I’ll be forced to start over somewhere I never thought I’d live.” When we are kids, our dreams are rose-colored. We picture an ideal future, and we cling to that dream as if holding on tight enough will make it come true.
The reality, though, is much harder. And when life doesn’t go as planned, it can feel like the ground is shifting beneath your feet. But what I’ve discovered is that sometimes the detours and the interruptions end up being the things that lead us toward growth, opportunity, and unexpected joy.
During my final year of college, my parents called me with news that stopped me in my tracks.“ We’re moving out of New York,” they said, “and heading to Ohio.” At first, I thought I had misheard them. Ohio wasn’t in my plans. Ohio wasn’t even on my radar. I had always pictured myself in New York. It was home to me. To suddenly be told that home was moving to a state I had barely thought about
was a shock – and not a pleasant one.
To be honest, the idea terrified me. I had always considered moving to a completely unfamiliar place a scary idea. The thought of starting over somewhere I had never envisioned myself permanently felt like losing a piece of my identity. And yes, I’ll admit, my first thought was, “Ohio? Of all places?”
My original plan was straightforward: graduate, move back home to New York, and start my job search there. That felt safe. That felt right. But suddenly, the “plan” was ripped away, and in its place was a big question mark. When I finally did make the move, the adjustment was hard. I didn’t love
it. The first few months, I resisted everything about Ohio. People encouraged me to try new things, to explore my new city, to meet new people. But I shut it all down. Ignoring their advice felt easier than dealing with the discomfort of change. So I stayed in. Weekends were spent avoiding the world. I told myself it was temporary. I’d figure out how to leave and how to get back to where I thought I belonged.
But here’s the thing: life doesn’t let you hide forever. Slowly, almost without realizing it, I started to inch out of my bubble. I met people. I discovered local spots. I dipped my toe into new hobbies. And to my surprise, something shifted. What once felt like a nightmare began to reveal its silver linings. I got involved in my community, made new friends, and even fell in love. These weren’t things I planned for or even thought were possible when I first got the news we were moving. But they happened.

Sometimes the things we fear most end up becoming blessings in disguise. Change is uncomfortable, but it also fixes us in ways we need. Had I stayed in my comfort zone, I never would have discovered this new version of myself, one who could adapt, grow, and still find joy even when life didn’t look the way I had imagined.
Of course, it wasn’t all sunshine and rainbows. There were plenty of days when I spiraled into negativity. When something felt unfamiliar or frustrating, my knee-jerk reaction was to complain. And honest-
ly, venting sometimes felt good. But over time, I noticed a pattern. The more I focused on the negatives, the heavier I felt. Negativity is like quicksand, the more you feed it, the deeper you sink. And the truth is, constantly complaining doesn’t just impact how you see the situation, it shapes how you see yourself.
I realized I had a choice: I could keep clinging to bitterness and resentment, or I could shift my energy toward something more productive. That didn’t mean pretending everything was per-


fect. It meant choosing to focus on growth and gratitude rather than letting negativity define me. Life-changing news, whether it’s a medical diagnosis, a sudden move, or some other curveball will shake you. It’s disorienting. It’s painful. But it doesn’t have to derail you.
When life doesn’t go as planned, you have two choices: Fight the change, stay bitter, and let it consume you. Or accept the change,
grow with it, and find the silver linings. Neither option is easy, but one of them opens the door to resilience and joy. I won’t pretend I’ve mastered this overnight. There are still days when I miss the life I thought I’d have. But the more I practice gratitude, the easier it becomes to see the good in the unexpected. Instead of focusing on what I lost, I remind myself of what I gained like new opportunities and new perspectives.
Maybe your story isn’t about moving to a new state. Maybe it’s about a diagnosis that changed your life, or a job loss, or a relationship that ended before you were ready. Whatever your detour looks like, you are not defined by the plan that didn’t work out. You are defined by how you grow and how you choose to keep going.

LFA,GOC BLOG & PODCAST
My Lupus Living Room

If you would like to share your story, or have a topic you think would benefit lupus patients, contact our show’s producer Alex by email: Alex@lupusgreaterohio.org
Check out our channel: @lupusgreateroh
Episode 49 - Brittney Refuses to Let Lupus Win Brittney embodies the definition of a lupus warrior. 556 Days. 6 different hospitals. Countless surgeries. A lot of people may have given up. She was determined to come home. Listen to her incredible story!
Episode 50 - A Family Overcoming Lupus Together
Melissa shares her incredible journey with lupus and how she, and her family, have managed to find strength together to overcome many hurdles along the way!
Episode 51- Tackling Lupus In Recovery
Valerie is a newly diagnosed lupus patient just beginning her journey. She shares her struggle to accept and understand her diagnosis while also in recovery from alcohol. Her story is a testament to strength, resilience, and perseverance.
Episode 52 - Seeking Community After Lupus Diagnosis
Jen Oster started getting a strange rash on her legs while recovering from COVID. After multiple doctors appointments, prescribed rounds of medication and testing she was diagnosed with lupus. Jen sits down with Suzanne to share what she went through along the way and ultimately how it changed her life forever.
Lupus Night Light
Our blog, Lupus Night Light, is a place where we share stories and practical advice from patients that they have learned along their lupus journeys. You will find stories of triumph, hardship, and everything in between. It is meant to be a cathartic journey for both the contributors and readers alike.

Email Sign-Up
Stay up-to-date on everything we’re doing by joining our mailing list. You will receive a monthly newsletter, support group reminders, Walk to End Lupus Now® updates, research news, and more. Sign up now: lupusgreaterohio.org/stay-informed
Text Message Notifications
Text “NOLUPUS” to 833-4490800, complete your contact information, and be sure to opt in to receive important lupus updates directly to your mobile device.
Get Social
Join us on our social media platforms to stay connected: lupusgreaterohio.org/stay-informed/ get-social
Instagram.com/lupusgreaterOH
Facebook.com/lupusgreaterOH
Twitter.com/lupusgreaterOH
Become a Member
One-year: $25 Lifetime: $200 lupusgreaterohio.org/get-involved
GET INVOLVED
Host a Third-Party Event
Do you have an idea to support the mission? Give us a call at the office to discuss and plan your own fundraising activity to benefit the LFA, GOC. Here are a few examples of virtual events that people have coordinated in the past: Pampered Chef Party, Online Auction, Charity Video Game Tournament.
If you are interested in hosting a third-party event, reach out to us for our official guidelines and an application.
Advocacy
Each year, the National Lupus Advocacy Summit brings together the lupus community to pursue a collective vision of a world without lupus. In addition, we help to ensure
there is a cohesive voice heard in Washington, D.C. that ensures the lupus agenda is at the forefront of the legislature. This year’s National Lupus Advocacy Summit will take place May 4-6, 2025 in Washington, DC. If you are interested in participating, please visit lupus.org for more information.
We invite you to register to be a lupus advocate in Ohio. Our current initiative is to keep lupus in the state budget for the new biennium. Much of the educational and support programming produced by the LFA, GOC over the past two years has been a direct result of the funding provided by the state of Ohio and the Ohio Department of Health. It is imperative that we let Ohio’s leadership know the importance of keeping lupus in the public health agenda. lupusgreaterohio.org/ get-involved/advocate
WAYS TO GIVE
Traditional
• Checks
Please make checks payable to the Lupus Foundation of America, Greater Ohio Chapter, and mail them directly to:
12930 Chippewa Road, Brecksville, Ohio 44141.
• Credit Card + PayPal
Fill out the online donation form or call the office.
• Facebook Fundraisers
• Instagram Stories
In Honor of
• Memorial Donation
• Tribute Donation
Through
Your Job
• Employer Matching Gift Program
Ask your employer if they match charitable contributions made by their employees.
• Combined Federal Campaign CFC #51890
Investing
• Stock or Other Securities
• Life Income Plans Pooled Income Fund Charitable Remainder Trusts
• Creating Healthier Communities CHC #9963
• United Way Campaigns
Other
• Donatestuff.com
Schedule a donation pickup of your gently used goods and pick the LFA, GOC as your charity.
• Leave a Bequest
You can include the LFA, GOC in your will to support the mission beyond your lifetime.
• Give the Gift of Life Insurance
Name the LFA, GOC as a sole or partial beneficiary.
For more information on ways to give, please visit: lupusgreaterohio.org/get-involved/ donate or call our office at 1 (888) NO-LUPUS.
Could You Have Lupus?
Lupus is a chronic autoimmune disease that causes inflammation in various parts of the body. The disease can range from mild to life-threatening. Ninety percent of those diagnosed with lupus are females between ages 15 and 44, but lupus also occurs in men, older people, and children. Lupus can be very hard to diagnose because symptoms vary from person to person, can come and go, and can mimic symptoms of other illnesses. is important to know the symptoms of lupus and to know if you are at risk for this disease. Here is a simple test to help you. Read each question and answer it in terms of your current AND past health.
Brain and Nervous System
Have you had a seizure or convulsion?
Have you had unexplained confusion that lasted more than an hour?
Have you had unexplained fever higher than 100º F/38º C for more than a few days that was not due to infection?
Heart and Lungs
Have you felt chest pain while taking deep breaths?
Have you had a stroke or heart attack?
Kidneys
Have you been told you have protein in your urine?
Have you had swelling in your legs and ankles on both sides at the same time?
Blood and Circulatory System
Have you been told you have anemia, low white cell count, or low platelet count?
Have your fingers and/or toes become pale or red or blue, or felt numb or painful?
Have you had blood clotting problems or a miscarriage?
If you have had any symptoms like these, especially if you have had several, talk to your doctor about lupus. Early diagnosis and proper medical care are the best ways to manage lupus.
Please turn over this page for more information.
Eyes, Nose, and Mouth
Have you had sores in your mouth or nose that lasted more than five days?
Have you developed irritation or dryness in your eyes or mouth for more than a few weeks?
Stomach and Intestines
Have you had unexplained weight loss or abdominal pain or tenderness when your belly is touched?
Muscles and Joints
Have you had stiff, tender, and swollen joints that feel worse in the morning?
Have you had extreme fatigue and weakness for days or weeks at a time, even after plenty of sleep?
Skin
Has your skin broken out after being in the sun, but it’s not a sunburn?
Have you had redness or rash across your nose and cheeks in the shape of a butterfly?
Have you had sores on your skin that would not heal?
Have you had sudden, unexplained hair loss?

Let's Talk About It Webinar Series
Living with Lupus Magazine
Lupus Night Light Blog
My Lupus Living Room Podcast
Patient Navigator Program
Educational Summits & Classes
Support Groups
Local State Advocacy Use this QR code to access program & educational resources.

The Lupus Foundation of America is the only national force devoted to solving the mystery of lupus, one of the world’s cruelest and devastating diseases, while giving caring support to those who suffer from its brutal impact. Through a comprehensive program of research, education, and advocacy, we lead the fight to improve the quality of life for all people affected by lupus. Contact the LFA or a chapter that serves your area to find out how you can become involved in our mission and how we can help you.
Suzanne Tierney, CEO/President Suzanne@lupusgreaterohio.org

Kathy Holmes Finance Manager
Kathy@lupusgreaterohio.org
I was diagnosed with lupus in 1989 and joined the Lupus Foundation of America, Greater Cleveland Chapter the same year. I have been able to grow with the organization, as it became the LFA, GOC. Knowing how important it was to have somewhere to turn when I was first diagnosed is what motivates me to do all I can to help our chapter continue in our mission. Being in remission for the past 20 years has enabled me to take an active part in the growth of our chapter.

Mackenna Willis Creative Design Manager
Mackenna@lupusgreaterohio.org
I’m the marketing manager and creative developer when it comes to strategizing new ideas for Lupus awareness. As a graduate from Bowling Green State University with a BFA in graphic design, I’ve always envisioned utilizing my skills to make a difference. My enthusiasm to help others through design has always been a passion of mine and having the opportunity to share and grow with the LFA, GOC team has been nothing but inspiring.
I have spent the last 30 years dedicated to the lupus patients in Ohio. The goal is to provide a better quality of life until a cause or cure for lupus is found. My passion is providing programs to empower those affected by lupus so that they will have a better journey with lupus through education and emotional support. Lupus does not have to be a lonely, miserable, and misunderstood illness. My goal is to provide my chapter with the tools and resources to provide such services to all those in the state of Ohio.
Rita O. Piccin, BS, ND, RN Lead Patient Navigator /Outreach Coordinator
Rita@lupusgreaterohio.org

chapter continue to grow and help lupus patients for years to come.
I am a caring, collaborative, and resourceful nursing professional with over 30 years of experience in a variety of roles. I have a BS in Biology and French from John Carroll University and a Doctor of Nursing degree from Frances Payne Bolton School of Nursing at Case Western Reserve University. I am passionate about giving effective and empathetic customer service and education to patients, caregivers, families, colleagues and community organizations. I am honored to be a part of the LFA,GOC and dedicated to providing education, support, and resources to lupus warriors.

Community Outreach Coordinator
Aletha@lupusgreaterohio.org
two wonderful sons, they are the reason I fight lupus daily. I share my story everyday hoping that it might help or encourage someone else on their journey. I try to leave lupus patients with these thoughts and that is keep your environment positive in all aspects and do what you can

Chris Milazzo Event Assistant
Chris@lupusgreaterohio.org
Helping others has always been one of my greatest passions. After graduating from SUNY Oneonta with a degree in Media Studies, I knew I wanted to use my degree to do good. Being able to work for the LFA, GOC has been one of the most rewarding experiences in my career so far. It brings a smile on my face knowing that the work I do is able to help the lupus community of Ohio, and I hope to continue being a helping hand for the community.

LIVING WITH LUPUS MAGAZINE
Thank you for reading Ohio’s Lupus Magazine! For the most up-to-date information from the world of lupus. Please visit us at www.lupusgreaterohio.org.
Lupus Foundation of America, Greater Ohio Chapter 12930 Chippewa Road, Brecksville, OH, 44141
Phone: (440) 717-0183
Toll-free: 1 (888) NO-LUPUS
